What Else Can Help
Whether you are suffering from patellofemoral arthritis or are recovering from surgery, exercises are really important to build up the strength and stability of the knee. Visit the knee pain exercises section for a whole range of strengthening and stretching exercises that can help.
If you want to know more about how arthritis affects the other parts of the knee, including the causes, symptoms, diagnosis and treatment options, visit the knee arthritis section.
Related Articles
What Does Arthritis In The Knee Feel Like
Millions of Americans suffer from chronic or acute knee pain every year.
Getting a proper diagnosis and receiving the needed treatments can be difficult without knowing the cause of your pain.
Many conditions can mimic one another, so its important to seek a medical professionals advice if you have been battling knee pain.
Arthritis is a prevalent cause of knee pain, and there are a few ways to tell if arthritis is causing your pain.
In the article below, we will answer the question: what does arthritis in the knee feel like?
Arthritis is the inflammation of one or more of your joints.
Joint pain, swelling, and stiffness are the main symptoms of arthritis.
Arthritis can affect any joint in your body, but your knee is particularly vulnerable.
Having arthritis in your knee can make it difficult for you to perform everyday activities, like climbing stairs or walking to the mailbox.
While there are many types of arthritis, the most common types of arthritis are osteoarthritis and rheumatoid arthritis.
Osteoarthritis is the most common form of knee arthritis.
Knee osteoarthritis is a degenerative disease caused by wear and tear.
Its the most common type of arthritis that occurs most often in people over 50, although younger people can get it as well.
The cartilage in your knee joint gradually wears away, and as it wears away, it becomes frayed and rough, and the protective space between the bones decreases.
When To Seek Treatment For Signs Of Arthritis
If unexplained joint pain persists or worsens, it is time seek the experience of a trained medical professional. It is common to begin the treatment process by making an appointment with a primary care physician, who may refer the patient to an arthritis specialist, called a rheumatologist.
A physician may recommend using arthritis pain relief creams, such as JointFlex, oral medications, joint injections, or perhaps weight reduction based upon the early warning signs of arthritis. However, its important to remember that a prompt diagnosis can help preserve joint function and mobility for many years to come.
Don’t Miss: Cellulite On Knees
Preventing Arthritis Of The Knee
How Do I Know If I Have Osteoarthritis
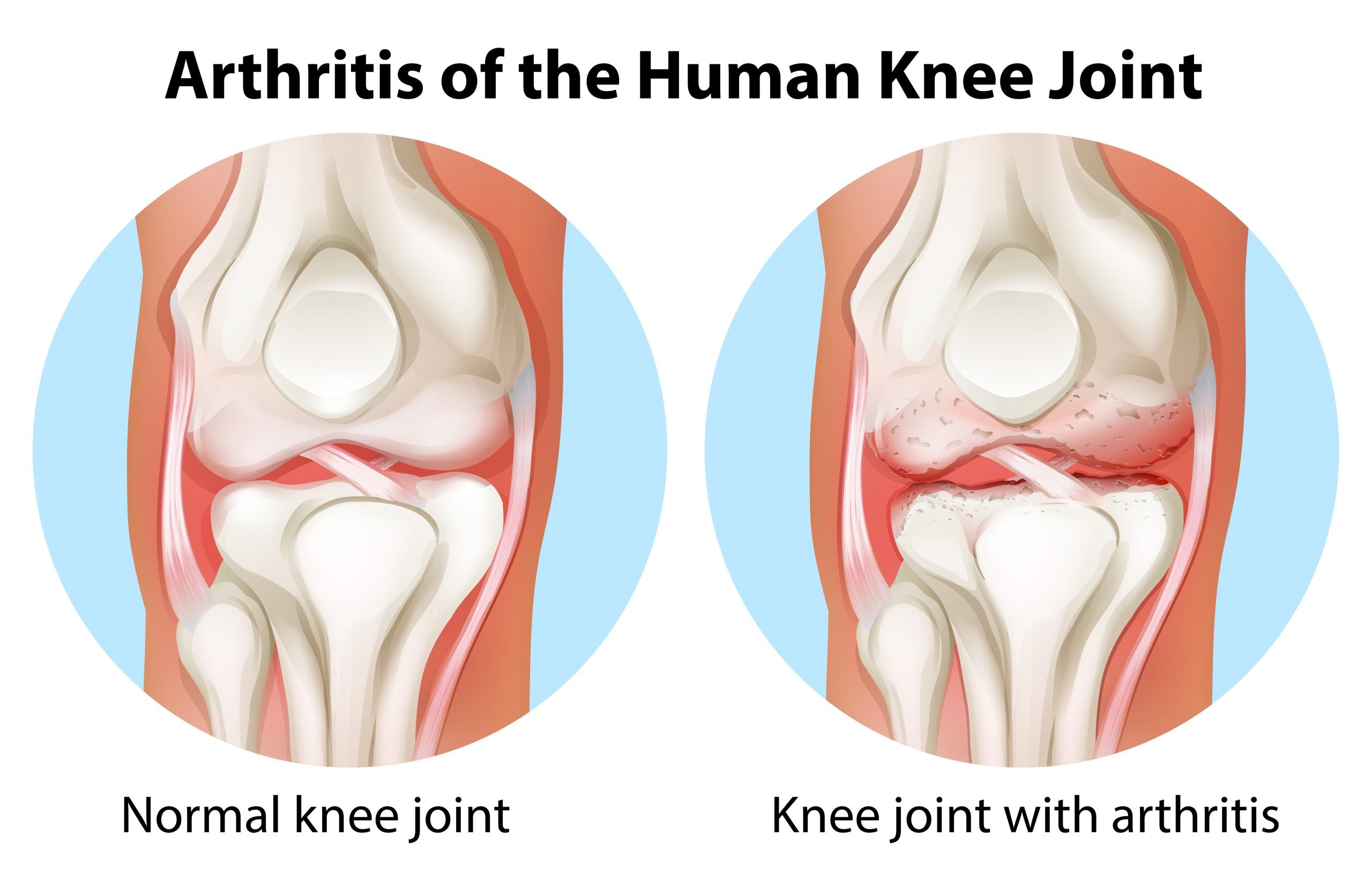
Unlike other types of arthritis, the pain from osteoarthritis usually develops gradually over many months or years. Often it increases with activities that put stress on the joint, such as running or prolonged walking. Pain and joint swelling tend to increase slowly over time. Sometimes, especially in more advanced disease, a sensation of crunching or grinding may be noticed in affected joints. Prolonged morning stiffness is not a prominent symptom in OA as compared to inflammatory arthritides, such as rheumatoid or psoriatic arthritis. Osteoarthritis does not usually cause fevers, weight loss, or very hot and red joints. These features suggest some other condition or type of arthritis.
Your healthcare provider can typically diagnose osteoarthritis by obtaining a complete history of your symptoms and examining your joints. X-rays may be helpful to make sure there is no other reason for the pain. Magnetic resonance imaging is generally not needed except in unusual circumstances or in cases when the cartilage or surrounding ligament tear is suspected. There are no blood tests that diagnose osteoarthritis. If a joint is particularly swollen, a doctor may need to drain fluid from that joint. Tests can be performed on the fluid to look for clues for other types of arthritis, such as gout.
Read Also: How Long After Knee Replacement Can You Fly
Knowing If You Have Arthritis Of The Knee
Treating Arthritis Of The Knee
Read Also: Inversion Table Knee Pain
How To Tell If You Have Arthritis In Your Knee
Millions of Americans suffer from chronic or acute knee pain each year, and it can be difficult to get appropriate treatment and much-needed relief without knowing the actual cause of the pain. Since many conditions can have symptoms that mimic one another, it is important to seek the advice of a professional when seeking a diagnosis, treatment, or therapy for your knee pain. Dr. Christopher Williams and the knowledgeable team at Interventional Orthopedics of Atlanta are highly experienced in assessing a vast array of bone, joint, and muscle symptoms and are dedicated to helping patients determine the cause of their pain and realize quick, effective, and long-lasting relief.
While Oa And Inflammatory Arthritis Do Share Some Symptoms Namely Pain Tenderness And Swelling The Similarities Tend To End There
If you have persistent knee joint pain, arthritis in your knees could be the culprit. While many forms of arthritis exist, its usually fairly easy for your doctor to first determine which of the two main categories osteoarthritis or inflammatory/autoimmune arthritis you might have.
Those include whats known as mechanical knee arthritis or inflammatory/autoimmune knee arthritis, which includes a number of illnesses such as rheumatoid arthritis , psoriatic arthritis, and ankylosing spondylitis.
While OA and inflammatory arthritis do share some symptoms namely pain, tenderness, and swelling the similarities tend to end there, as youll see below. The answers to the following questions can often help determine if your knee pain is osteoarthritis or inflammatory arthritis.
Don’t Miss: How To Remove Scar Tissue From Knee Surgery
What Are The Risk Factors For Osteoarthritis
In addition to age and secondary causes such as inflammatory arthritis and prior injury/ trauma, several other risk factors increase the chance of developing osteoarthritis including obesity, diabetes, elevated cholesterol, sex, and genetics.
- Obesity is a risk factor for osteoarthritis, particularly of the knee. In addition to overloading the weight-bearing mechanisms of the body, the metabolic and pro-inflammatory effects of obesity have been studied as contributory to osteoarthritis. Maintaining ideal body weight or losing extra weight is important for those at risk.
- Both diabetes and hyperlipidemia contribute to the inflammatory response within the body, increasing the risk of osteoarthritis. Oxidation of lipids can also create deposits in cartilage which affects affecting blood flow of subchondral bone in the same way that blood vessels are affected by atherosclerosis. Elevated blood sugars, as well as elevated cholesterol/lipids, increase free radicals within the body, this oxidative stress exceeds the resilience of cartilage on the cellular level. Controlling diabetes and hyperlipidemia is important for bone health in addition to general health.
- Heredity can play a role in osteoarthritis, as individuals born with other bone diseases or genetic traits may be more likely to develop osteoarthritis. For example, Ehlers-Danlos, which is characterized by joint laxity or hypermobility, can contribute to osteoarthritis.
Risk Factors You Can Control
Because injured joints are more vulnerable to osteoarthritis, doing anything that damages the joints can raise your risk. This includes sports that have a high rate of injury and jobs that require repetitive motion, such as bending the knees to install flooring. Obesity is another risk factor — it has been linked specifically to osteoarthritis of the hands, knees and hips.
Don’t Miss: How To Prevent Knee Pain In Old Age
Limited Mobility Or Range Of Motion
For men and women who develop arthritis in their knees, activities that were once simple, easy, or routine may become difficult or even impossible to do without limitations and discomfort. Walking, running, or getting in and out of a car can, oftentimes, prove disproportionately challenging for patients with arthritis of the knee. The damage and loss of cartilage associated with arthritis are usually to blame for this phenomenon.
What Does This Mean For My Lifestyle And Quality Of Life
The impact of severe arthritis on quality of life is different for all people and there are many factors that help determine this. The severity of symptoms is one of the main factors in the impact of arthritis on your quality of life. If someone experiences less impacted mobility and less pain in general, their lifestyle would typically be affected to a lesser extent. Staying proactive when possible in trying to reduce the impact of various everyday activities can go a long way in maintaining your lifestyle. Working with a medical professional to find a suitable management plan for you, as well as being careful to follow that plan can also help to maintain quality of life. In this section, we will discuss some of the common challenges in the day-to-day life of someone impacted by late-stage knee arthritis.
Difficulty Squatting
As mentioned earlier squatting places forces on the knee that are many times greater than a persons body weight. In advanced arthritis, this makes it much more difficult to squat due to the pain and stiffness in the affected joints. This can make performing household tasks, exercises or working more difficult.
You May Like: How To Whiten Knees And Elbows
What Symptoms Look And Feel Like And What To Do If You Can’t Shake The Ache
by Michelle Crouch, AARP, February 18, 2020| 0
En español | It’s not unusual to experience pain in your joints on occasion, especially if you’re active and participate in high-impact activities such as running. That unwanted ouch can be caused by injured muscles, tendons and ligaments around the joint, by tendonitis or by a sprain or a strain.
But if you start experiencing aching, pain and stiffness on a routine basis and particularly if the pain is right at the joint you may be developing arthritis, says rheumatologist Uzma Haque, codirector of clinical operations at the Johns Hopkins Arthritis Center in Baltimore.
“The cardinal feature of arthritis is a swollen joint, Haque says. However, pain, discomfort and stiffness can be early signs.”
Haque recommends paying attention to what triggers your symptoms: If you walk a block and consistently have aching in your right knee, but it improves when you sit down, that’s when you should think, Do I need a medical evaluation?
And yes, you might need to book that appointment even if you’re well under 50. Arthritis doesn’t only affect older people. Although your risk increases as you age, more than half of arthritis patients are younger than 65, according to the Centers for Disease Control and Prevention . It’s a leading cause of disability in the U.S., affecting around 54 million people.
Who Is Affected By Osteoarthritis
Approximately 80% of older adults, ages 55 years and older, have evidence of osteoarthritis on X-ray. Of these, an estimated 60% experience symptoms. It is estimated that 240 million adults worldwide have symptomatic osteoarthritis, including more than 30 million U.S. adults. Post-menopausal women have an increased incidence of knee osteoarthritis compared to men.
Recommended Reading: Scar Tissue After Knee Arthroscopy
Osteoarthritis: What Is It
Also called “wear and tear” arthritis or degenerative joint disease, osteoarthritis is the progressive breakdown of the joints’ natural shock absorbers. This can cause discomfort when you use the affected joints — perhaps an ache when you bend at the hips or knees, or sore fingers when you type. Most people over 60 have some degree of OA, but it also affects people in their 20s and 30s.
Early Signs Of Arthritis
While some signs of arthritis develop and worsen with time, other symptoms are often present at the onset of the disease. Common early signs of arthritis are morning stiffness,4 fatigue,5tingling,6 and numbness of the joints.
Individuals with early onsite arthritis may feel unusually fatigued doing normal daily activities, and this fatigue may come or go on certain days. Tingling and numbness may be mild sensations in the beginning. Stiffness in the morning that only lasts a few minutes is often an early warning sign of a degenerative form of arthritis, such as osteoarthritis. Meanwhile, individuals who experience morning stiffness that lasts a few hours may be feeling an early warning sign of rheumatoid arthritis or another form of inflammatory arthritis.6
Also Check: How Do You Get Rid Of Scar Tissue After Knee Replacement
Are There Different Types Of Knee Osteoarthritis
The knee has three contact zones, also known as compartments where osteoarthritis usually occurs. A common way to classify knee osteoarthritis is by which of the three compartments of are affected:
- Medial Tibiofemoral Compartment the inside part of the knee where the tibia meets the femur .
- Lateral Tibiofemoral Compartment The outside part of the knee where the tibia meets the femur .
- Patellofemoral compartment The front of the knee between the patella and femur .
Estimates of how common osteoarthritis is in each compartment of the knee vary quite widely. A study published by Oxford University found that of a group of subjects with radiographic knee osteoarthritis :
- 59% had osteoarthritis in both the patellofemoral compartment and at least one tibiofemoral compartment.
- 35% had osteoarthritis only in the patellofemoral compartment
- Only 6% had osteoarthritis in one or both of the tibiofemoral compartments.
How Is An Mri Used To Diagnose Osteoarthritis
A radiologist may perform an MRI of a joint with possible osteoarthritis if X-rays are inconclusive. The doctor may also want to look for possible tears and strains in other tissues surrounding the joint.
During the visit, the MRI technician will ask you to lie on a table. He or she will then move the table into the MRI machine, so that the injured area is in the machine. This means that if your shoulder is being looked at, only the top half of your body will need to be in the machine. Your MRI results will then be sent to your doctor, who youll see at a follow-up appointment.
When examining an MRI, an orthopedist will typically look for the following structures, which may indicate osteoarthritis:
- damage to the cartilage
- osteophytes, also called bone spurs
- subchondral sclerosis, which is increased bone density or thickening in the subchondral layer of the joint
- joint effusion, or excess swelling of fluid around the joint
- synovitis, which refers to inflammation of the synovial membrane in joints
- tears in ligaments, which may increase your risk for early osteoarthritis, or cause pain or impaired function
Before scheduling an MRI, your doctor will first review your symptoms and ask:
- your degree of pain
- how long youve had pain
- activities that are difficult because of your pain or decreased mobility
Your doctor will also perform a physical examination and look for the following:
Read Also: Inversion Table For Knee Pain