Does Medicare Part B Cover Hyaluronic Acid Injections
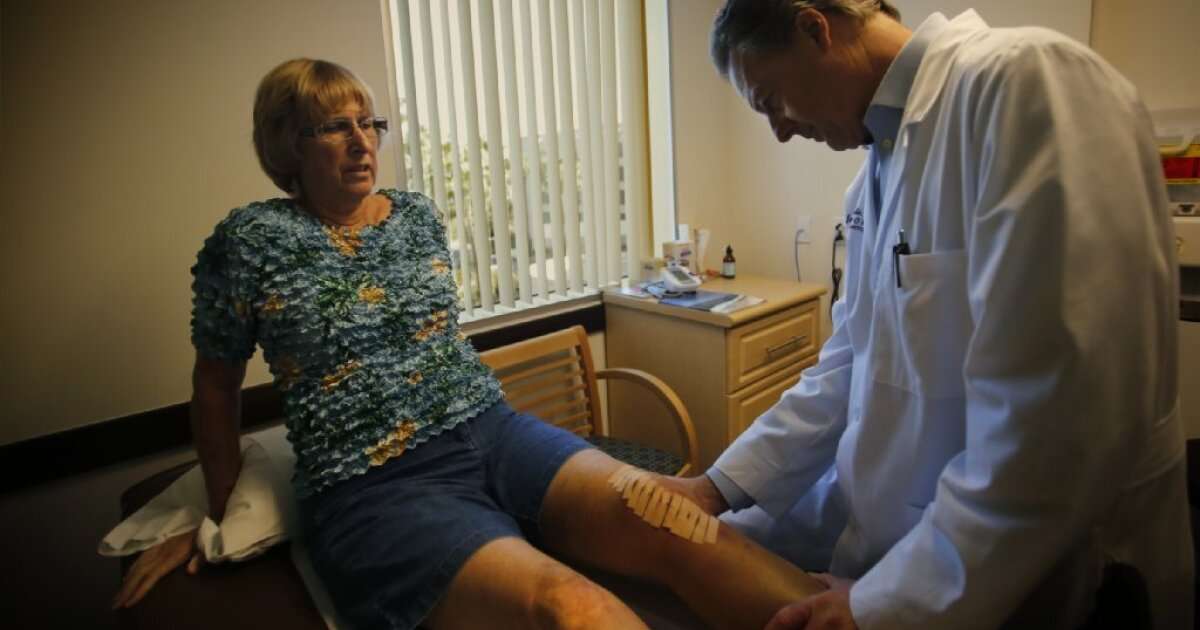
Medicare Part B may cover hyaluronic acid injections for the knee if you have symptoms of knee pain or stiffness that interfere with one or more daily living tasks like sleeping comfortably or standing for long periods of time. In addition, prior to coverage, your doctor must:
- Perform imaging tests and other diagnostic testing to rule out any other possible cause for your symptoms and confirm that you have osteoarthritis of the knee
- Try other treatments like physical therapy and over-the-counter pain relievers to manage your symptoms for at least three months
- Attempt to treat your symptoms by either removing fluid from your knee or prescribing corticosteroid injections
What Does Medicare Cover With A Hip Or Knee Replacement
Original Medicare Medicare Part A and Part B cover a wide variety of costs associated with hip and knee replacement surgery, also called lower extremity joint replacement or LEJR.
A Medicare Part D plan can help cover prescription drugs related to your hip or knee replacement surgery, while a Medicare Supplement plan helps cover the out-of-pocket costs not covered by Original Medicare.
Medicare Advantage plans must cover what Original Medicare does, but may include additional benefits.
Is Coolief Covered By Medicare
Medicare should cover Coolief treatment. Although, we recommend confirming with your doctor and insurance provider. This method of treatment doesnt require any incision, no overnight hospital stay, and pain relief can last up to 12 months.
Most patients report an increase in mobility. In the Coolief clinical study, they found the treatment was longer-lasting and gave greater pain relief than the steroid injections. However, there are risks to all medical procedures discussing your options with your doctor is very important.
Read Also: How Much Does Aflac Pay For Outpatient Surgery
Will Medicare Pay For A Total Knee Replacement
- Asked July 24, 2013 in
Contact Bruce McLean Contact Bruce McLean by filling out the form below
Bruce McLeanOwner, Better Benefits, Medicare is very comprehensive health coverage for those that qualify. Medicare will cover a Total Knee Replacement as long as the Physician, Hospital, and any other healthcare providers are deemed as providers. You can check each provider out on the Medicare.gov website. Medicare Part A would cover the hospital expenses and if a Skilled Nursing Facility is needed for rehabilitation. You will have a deductible if you only have Medicare A and B. A Medicare Supplement can cover all or part of the out of pocket costs. Medicare Part B would cover the Physician charges and any outpatient services required. You have an annual deductible and 20% coinsurance. A Medicare Supplement can cover all or part of these our to pocket cost.Medicare Advantage plans have daily charges and copays that vary for every plan. You should check with the plan to confirm that the providers are in their network and determine what your costs might be.Answered on July 24, 2013+24
Read Also: Is Dexcom G6 Cgm Covered By Medicare
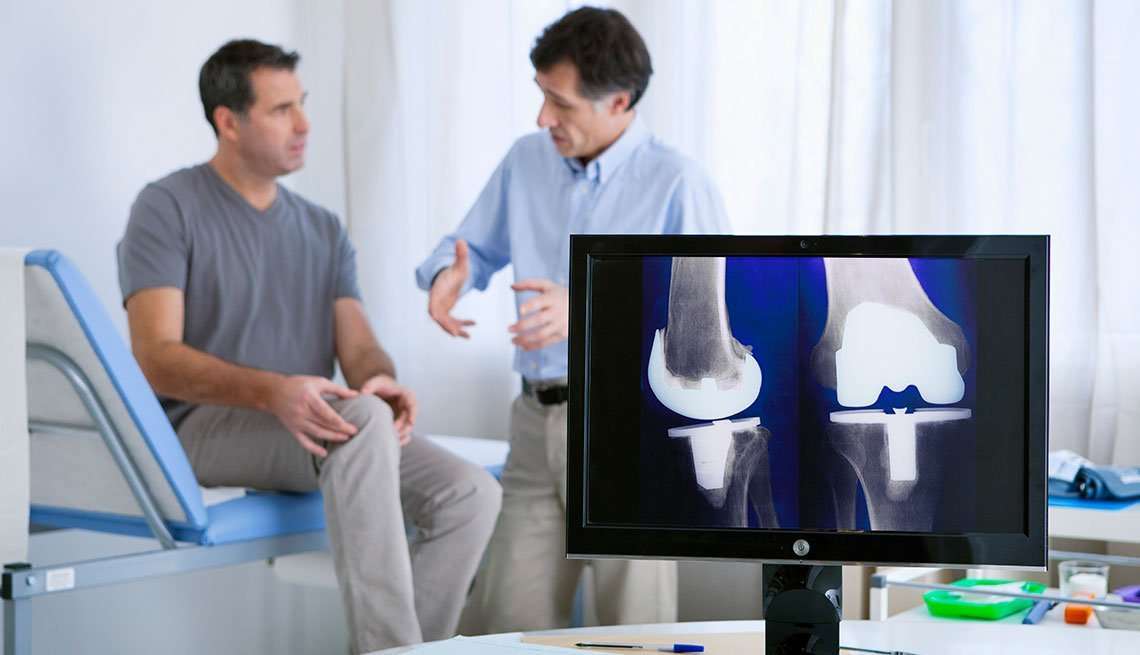
What Do You Need To Know About The Cost Of Knee Replacement Surgery
The average hospital charge for a total knee replacement in the United States is $49,500. A partial knee replacement typically costs about 10 to 20 percent less than a TKR. The main reason is that the operation requires a shorter hospital stay: an average of 2.3 days, compared to 3.4 days for a TKR.
Donât Miss: How Old To Get Medicare And Medicaid
Don’t Miss: How To Whiten Knees Fast
What Does This New Medicare Rule Mean
- The new Medicare rule represents a recognition that patients often recover from surgery better in their own homes and that extensive hospital stays are no longer required for post-operative rehabilitation.
- Hip and knee replacement surgeries were previously on the Inpatient-only list of procedures that typically require patients to stay in a hospital overnight after surgery. These surgeries are now classified as outpatient, meaning the patient is expected to stay in the hospital for less than 24 hours.
- This gives patients more options in choosing the location, quality of care and the ability to save in the cost of their care.
C Coverage For Rehab After Knee Surgery
Medicare Advantage plans also provide coverage for rehabilitation after knee surgery. Part C plans are required to cover all the same treatments, procedures and services that Parts A & B cover. But Part C plans will also include coverage for things that Parts A & B do not. Exactly what those things are and how much they cost depend on the Part C plan you have.
Read Also: Inversion Table Knees
Understanding The Hip Replacement Procedure
Hip arthroplasty, also known as total hip replacement, is a common orthopedic procedure. During the surgery, your damaged bones and some soft tissue are removed.
The hip joint is replaced with an implant, which can be ceramic, plastic, or metal.
In a traditional replacement, a 10-12 inch incision is made on the side of the hip. In less-invasive procedures, the incision may only be three to six inches.
Some people may not be eligible for a minimally invasive procedure. Be sure to ask your doctor if you arent sure what your procedure will be like.
Also Check: Best Knee Walker 2016
How Do You Proceed Once Your Parent Has A Doctors Signed Prescription For A Dme
As long as Medicare Part B is satisfied that your parents DME is medically necessary, they will cover 80% of theMedicare-approved price for the DME.
Your parent will then be responsible for paying their Medicare 20% co-payment of the Medicare-approved price of the DME, as long as they have used a Medicare-enrolled participating supplier who accepts assignment.
If not, your parent may owe much more !
Your parent will also have to pay their deductible, if it hasnt already been met.
Also Check: Inversion Table Knee Pain
What Should I Consider In Knee Surgery Cost After I Am Discharged From The Hospital
You may be sent home with prescription medications to manage pain, and reduce the risk of blood clots or infection. You will probably have one or more follow-up appointments with your surgeon. You may also need physical therapy or other rehabilitation services for a few weeks after the procedure.
Although there is generally no coverage under Original Medicare for prescription medications you take at home, Part B typically pays 80% of allowable charges for all medically necessary doctor visits and physical or occupational therapy services you need after your surgery. Part B usually also generally covers durable medical equipment such as a cane or walker if your doctor orders one for you to use during your recovery. Itâs a good idea to discuss your after-surgery care with your doctor so you know what to expect and can better plan for your out-of-pocket expenses.
In some cases, your doctor may recommend a brief stay in a skilled nursing facility after your knee replacement. In order to be eligible for Part A skilled nursing facility coverage, you must have a qualifying hospital stay of at least three days prior to your admission. If your stay is covered, you pay nothing for the first 20 days of skilled nursing facility care there is a daily coinsurance amount applied to days 21 and beyond.
Do Different Surgeons Charge Different Amounts For Knee Replacements
Medibank and the Royal Australasian College of Surgeons research has found that patients needing a knee replacement could potentially incur thousands of dollars more or less in medical costs than other patients, depending on their choice of surgeon. The research showed the average total cost of a knee replacement including Medicare rebates, as well as out-of-pocket costs, varied by more than $12,000, based on a wide dataset.
Also Check: How Old To Be Eligible For Medicare
Read Also: Ginger Poultice For Knee Pain
What Is Your Out
While Medicare covers much of the cost for approved hip or knee replacement, you will still have to pay deductibles, copayments and coinsurance.
The amount you owe will depend on the type of Medicare coverage you have.
Your Medicare Out-of-Pocket Costs for Knee or Hip Replacement Surgery
- Medicare Part A
- You are responsible for paying your Medicare Part A deductible $1,556 for each benefit period in 2022. The benefit period begins the day you are admitted to a hospital and ends after you have not been readmitted for 60 days in a row.
- Medicare Part B
- You will still have to pay 20 percent of the Medicare-approved cost of the medical device and other medical services. Your Medicare Part B deductible $233 in 2022 also applies.
- Medicare Advantage Plans
- The amount varies from plan to plan. You should contact your Medicare Advantage plan administrator to find out how much you will have to pay.
- Medicare Part D
- Your out-of-pocket costs will vary from plan to plan. You should check with your plan administrator to find out your share of the costs. You should also ask your doctor about alternative drugs on your Medicare Part D formulary that may cost you less.
Read Also: How To Get Rid Of Knee Fat And Cellulite
American Hospital Association Disclaimer
The American Hospital Association has not reviewed, and is not responsible for, the completeness or accuracy of any information contained in this material, nor was the AHA or any of its affiliates, involved in the preparation of this material, or the analysis of information provided in the material. The views and/or positions presented in the material do not necessarily represent the views of the AHA. CMS and its products and services are not endorsed by the AHA or any of its affiliates.
Read Also: Best Knee Walker 2016
How Does Medicare Cover Knee Replacements
Getting a knee replaced requires surgery. And since Medicare only covers surgical procedures that are deemed medically necessary, your knee replacement surgery must be deemed medically necessary by your doctor for Medicare to cover it.
Which part of Medicare actually covers your surgery depends on what kind of surgery you get. If your knee surgery is in an inpatient procedure, Medicare Part A will provide coverage. If you get outpatient surgery, Medicare Part B would provide coverage. If you have a Medicare Advantage plan, your coverage may be different as well. Talk with your plan provider for specifics.2
Your costs will vary based on the type of procedure you need and your Medicare coverage. If Medicare covers your surgery, you still likely will have costs including a deductible and coinsurance.
What Other Medicare Benefits Are Available For Knee Surgery Cost
A pays some or all of your out-of-pocket knee replacement costs under Part A and Part B, except for your premiums. Depending on the plan you choose, your Medicare Supplement Plan may cover your Part A and Part B deductibles and coinsurance amounts. Keep in mind, however, that Medicare Supplement Plans generally do not cover any out-of-pocket costs associated with prescription drugs not covered by Medicare.
is how Medicare beneficiaries get prescription drug coverage. Medicare Advantage plans and stand-alone Medicare Part D Prescription Drug Plans are offered by private insurance companies, which means that plan benefits, deductibles, and cost-sharing structures may vary widely from plan to plan. Each plan may treat knee replacement cost and associated expenses a bit differently. Read your plan documents carefully before your procedure to help you estimate your out-of-pocket knee surgery cost.
If you are covered by a Medicare Part D Prescription Drug Plan, either as a complement to Original Medicare or as part of a Medicare Advantage plan, the medications you take at home are generally covered. You may have a deductible, copayment, or coinsurance amount for these medications.
Don’t Miss: Flying After Knee Replacement Surgery
What Equipment Does Medicare Cover
For use in the home, Original Medicare Part B covers durable medical equipment which must
- be able to withstand repeated use over a sustained period of time durable
- be used for a medical reason only not for comfort
- be of use to someone who is actually sick, and of little use to a person who is well
- be primarily for use in the home
- be expected to last at least 3 years
Donât Miss: Scar Tissue Removal Knee Surgery
Medicare Now Covers Outpatient Total Joint Replacement Surgery
Beginning in 2020, Medicare will cover outpatient total joint replacement under the Center for Medicare & Medicaid Services new Hospital Outpatient Prospective Payment System & Ambulatory Surgical Center Payment System Rule.
In the past, total joint surgeries have required extended stays in the hospital or a rehab facility while the patient recovers. Now, better anesthesia techniques, surgical techniques, and improvements in prosthetic implants have significantly reduced the recovery time after a joint replacement. This means that extensive hospital stays are no longer required for post-operative rehabilitation.
Find out what this new rule means for you, and if you are a candidate for outpatient joint replacement.
Also Check: How Much Does Aflac Pay For Ambulance Ride
She Was A Victim Of The Medicare 3
The 3-day rule is Medicares requirement that a patient has to be admitted to the hospital for at least 3 days in order for Medicare to cover the cost of a SNF after the hospitalization. If the patient is admitted for less than 3 days, then the patient pays the cost of the SNF and Medicare pays nothing. So, if this patient was in the hospital for 4 days, why didnt Medicare cover the cost of the SNF?
It all has to do with when the inpatient stay clock starts and that has nothing to do with when the patient first comes into the hospital for a surgery or a medical condition. It solely depends on when the attending physician entered an order for that patient to be in inpatient status as opposed to observation status. Medicare considers a patient to be in inpatient status if that patient is anticipated to need to be in the hospital for 2 midnights and in observation status if the patient is anticipated to be in the hospital for less than 2 midnights. Observation status was originally intended to be used to observe the patient to determine whether the patient is sick enough to warrant being admitted to the hospital.
Bluewave Insurance Is Here To Help
So, does Medicare cover for knee gel injections? Yes, Original Medicare does pay for knee gel injections. However, that doesnt mean that everyone with Medicare coverage qualifies.
You will still need to show proof that you have osteoarthritis, and that other treatments have been ineffective. Even though Medicare covers part of the costs, you may still need help paying for drugs, deductibles, or copayments as well. This is where an MAPD or Medigap insurance plan with Bluewave Insurance can help.
thumb
If you have any further questions about Medicare or want to learn more about cost-sharing Medigap options, call us attoday!
Read Also: Does Aflac Pay For Sprains
Does Medicare Cover Knee Replacement Costs
In general, Medicare only covers procedures that are medically necessary. According to the Centers for Medicare & Medicaid Services, doctors need to document whether the knee replacement surgery is medically necessary.
Before you have the surgery, you may want to find out if Medicare will cover your knee replacement costs in your situation. Ask your doctor:
- Is the surgery medically necessary?
- Will it be inpatient or outpatient surgery?
- How much will it cost me?
You may also want to contact Medicare to see if the knee replacement costs will be covered in your situation. You can reach a representative 24 hours a day, seven days a week, at 1-800-MEDICARE .
Even if Medicare covers your surgery, you may have to pay a deductible and/or coinsurance amount.
How Can A Medicare Supplement Plan Help

While a Medicare Advantage plan may cover most of the costs, you may want to consider a Medicare Supplement plan. Medicare Supplement helps cover costs that Original Medicare doesnt cover. More specifically, a Medigap plan will allow you to see ANY doctor, anywhere in the country that accepts Original Medicare.
For example, if you need gel shots once every six months, you might not meet your deductible in time. A Medigap plan can help pay your deductible, ensuring that Part B covers the injections. This could also save you money on other knee treatments covered by Medicare.
Read Also: Dcf Knee Compression Sleeve
Should Medicare Allow Outpatient Knee Replacement
Medicare Part A does not cover outpatient surgical costs. Instead, Medicare Part B provides coverage. Most people receive knee replacement surgery on an inpatient basis. However, Medicare also covers outpatient knee replacement surgery, where an individual stays in a medical facility for less than 24 hours.
Also Check: What Age Do You Draw Medicare
Medicare Covered Alternatives To Knee Replacement Cortisone And Pain Meds
If the prospect of having knee replacement surgery isnt exactly high on your list of things to do, you will be happy to know that there are alternatives. Unfortunately, the challenge people often have is that not all of them are covered by insurance.
If you are like most people who need to have knee replacement, there is a good chance that you have Medicare. This is because, according to Healthline, the average age of people having the surgery is 70.
So,if you are looking to avoid knee replacement surgery and the risks that come along with it, you can try these three options that are covered by Medicare to see if you can get better results.
You May Like: Nano Knee Cost