How Much Does Medicare Pay For Hip Replacement Surgery
The likelihood of needing hip replacement surgery increases with age. Seniors 65 and older, people with ALS or ESRD, or people who have received SSDI for at least 25 months qualify for Medicare.
Original Medicare will help cover the cost of hip replacement surgery if your doctor determines its medically necessary because other treatments have failed. The answer to how much Medicare pays for hip replacement surgery will depend on whether it is medically necessary and what types of coverage you have.
What Should Be Included In The Cost
Prior to surgery, your orthopedic surgeon should carry out an evaluation of your knees present strength and range of motion, and make the determination of whether total knee replacement surgery is the best course of action.
If your surgeon decides to proceed with the operation, there are a number of services that should be included in the cost. Anesthesia, perhaps the most important part of any surgical procedure, is included in the cost at almost every hospital. For total knee replacement, general or epidural anesthesia is usually required.
While you are under anesthesia, the orthopedic surgeon will remove your damaged bone and cartilage, and insert artificial joint surfaces made of plastic and metal. The cost of the knee replacement device itself will also be included in the total cost of your surgery. There are a number of different knee replacement device manufacturers, with different products used depending on the hospital and your particular condition. Two of the more common device manufacturers are Zimmer and Stryker.
After surgery, you will be required to stay in the hospital for several days for initial recovery from your knee replacement. Your hospital bill may or may not include the cost of preliminary physical therapy and rehabilitation sessions.
Understanding The Hip Replacement Procedure
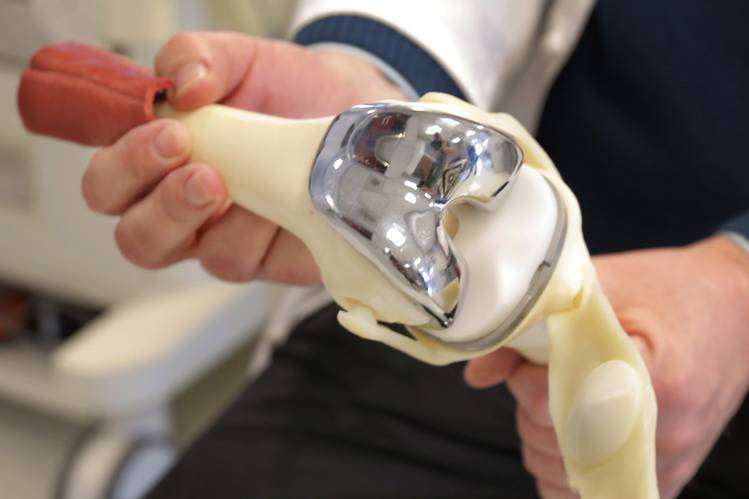
Hip arthroplasty, also known as total hip replacement, is a common orthopedic procedure. During the surgery, your damaged bones and some soft tissue are removed.
The hip joint is replaced with an implant, which can be ceramic, plastic, or metal.
In a traditional replacement, a 10-12 inch incision is made on the side of the hip. In less-invasive procedures, the incision may only be three to six inches.
Some people may not be eligible for a minimally invasive procedure. Be sure to ask your doctor if you arent sure what your procedure will be like.
Read Also: How Do I Get Rid Of Fat Around My Knees
Find Medicare Advantage Plans That Cover Knee Replacements And More
Because Medicare Advantage plans must offer the same benefits as Medicare Part A and Medicare Part B, your Medicare Advantage plan should cover your knee replacement surgery if a doctor says it is medically necessary.
If youre eligible for Medicare enrollment or are interested in changing to a Medicare Advantage plan, call a licensed insurance agent today to see what Medicare Advantage plans are available in your area.
Find Medicare Advantage plans that cover knee replacement
Or call to speak with a licensed insurance agent. We accept calls 24/7!
1 Ubel, Peter. Medicare Is Reducing The Cost Of Knee Replacements . . Forbes. Retrieved from www.forbes.com/sites/peterubel/2017/02/10/medicare-is-reducing-the-cost-of-knee-replacements-heres-how-that-could-backfire/#279a55416392.
2 BlueCross BlueShield. . Planned knee and hip replacement surgeries are on the rise in the U.S. Retrieved from www.bcbs.com/the-health-of-america/reports/planned-knee-and-hip-replacement-surgeries-are-the-rise-the-us.
About the author
Christian Worstell is a licensed insurance agent and a Senior Staff Writer for MedicareAdvantage.com. He is passionate about helping people navigate the complexities of Medicare and understand their coverage options.
His work has been featured in outlets such as Vox, MSN, and The Washington Post, and he is a frequent contributor to health care and finance blogs.
Where you’ve seen coverage of Christian’s research and reports:
Does Medicare Cover Continuous Passive Motion Devices
For those of you who have parents who need total knee replacement surgery, Medicare Part B will cover the use of CPM devices for total knee replacements, or for the revision of a previously performed total knee replacement.
CPMs are not covered for any other kind of knee surgery by Medicare Part B.
The Medicare coverage is only for the 21 days from the date of surgery.
You May Like: When Can I Shower After Knee Replacement Surgery
What Is The Cost Of Knee Replacement In Other Countries
For American patients without health insurance, it might be worth considering medical tourism, i.e., leaving the country for knee replacement surgery. Many countries in the world offer this procedure for costs dramatically lower than those in the United States. We have listed knee replacement cost estimates from various medical tourism destinations in the chart below. The cost of total knee replacement surgery will also vary from patient to patient, depending on factors such as age and medical history.
Other Funding Your Loved One Can Get For Ice Machines Or Cold Therapy Units
These are programs which help to increase access to assistive devices in the home.
The elderly are one of the primary focuses.
DME and Assistive Technology are very interchangeable as terms, so participants are able to get a wide range of different medical devices to help them in their homes.
To find out what programs your state runs click here.
Read Also: Dcf Compression Knee Sleeve
The Best Plan: Weight Loss Low
The better plan is to begin by increasing low-impact exercise, like swimming and biking, and slowing down on running and other exercise that puts more pounding on the knee joints, said Eric Mirsky, director of orthopedic surgery at Summit Medical Group in Berkeley Heights, New Jersey.
Practicing doctors are also pushing to squeeze out the unnecessary care because of the rising importance of value-based care reimbursement, which rewards doctors for delivering better results rather than performing more procedures, Mirsky said. “We want to know if we’re giving the most bang for the buck,” he said.
But doctors continue to push the limits of when the surgery is appropriate, sometimes in cases where knees locking, a symptom surgery can fix, coincides with more subtle signs of degeneration, Mirsky said.
So what should patients do?
First, ask themselves honestly whether their symptoms are coming more from their arthritis or their cartilage damage, Mirsky said. Physical therapy, cortisone injections and losing weight are all better, less-expensive strategies when most of the problem is arthritis.
More from Modern Medicine:
The Type Of Knee Replacement You Need
There are three types of knee surgeries, each with varying levels of complexity and equipment needs:
- Partial knee replacement
- Total knee replacement
- Revision knee replacement
Your orthopedic surgeon will work with you to determine which type of knee replacement will work best for you. At TRIA, our orthopedic surgeons will coach you through the process, and make recommendations based on many factors, including: your age, knee health, bone structure, range of motion, lifestyle, goals and the possibility of needing a revision surgery in the future.
While it may seem a full knee replacement surgery would be the most costly, a revision surgery is actually the most expensive. Total cost of any surgery will depend on complexity of the surgery, among other factors, but a partial knee replacement typically costs anywhere from 10% to 50% less than a total knee replacement.
Also Check: How To Reduce Swelling After Total Knee Replacement
Other Costs That May Be Associated With Medicare Coverage Of Knee Replacement Surgery
Another possible cost you might want to plan for is that of any prescription medications your doctor might prescribe, such as painkillers, anticoagulants, or antibiotics. Medicare Part A may cover prescription drugs you receive as part of your inpatient treatment, while Medicare Part B may cover certain prescription drugs administered to you as an outpatient. But Original Medicare typically doesnt cover medications you take at home.
A stand-alone Medicare Part D Prescription Drug Plan may help cover your prescription drugs, although not every prescription drug is covered under every plan. Offered by private, Medicare-approved insurance companies, Medicare Prescription Drug Plans maintain their own formularies . If youre thinking about enrolling in a Medicare plan that includes this coverage, you might want to check the plans formulary before you enroll to make sure your prescriptions are covered. A plans formulary may change at any time. You will receive notice from your plan when necessary.
If you have other questions about Medicare coverage, or would like to learn more about your Medicare plan options that may give you more benefits, we would be happy to help. You can use the links below to request a phone call or an email containing personalized information. Of course, you can also shop Medicare plans in your area on your own by clicking the Find Plans button on this page.
New To Medicare?
How Much Does A Knee Replacement Cost With Medicare
The total cost of a knee replacement with Medicare is going to vary depending on your coverage. Remember that you have to meet your deductible first for services to be covered under Medicare. Your out-of-pocket costs are going to depend on your specific plan.
Check with your Medicare plan representative to find out more information about specific costs related to knee replacement surgery.
Also Check: How To Stop Limping After Knee Surgery
Does Medicaid Cover Ice Machines Or Cold Therapy Units
Medicaid is a very different beast from Medicare, and is funded both on a federal level and a state level.
The states have a lot of latitude in what they can do, as long as they stay with basic guidelines, and a lot of Medicaid programs for outside of skilled nursing care facilities have been developed.
One of the results of this, is that there are literally hundreds of different programs and waivers across the US, and which vary greatly from state to state.
Is Coolief Covered By Medicare

Medicare should cover Coolief treatment. Although, we recommend confirming with your doctor and insurance provider. This method of treatment doesnt require any incision, no overnight hospital stay, and pain relief can last up to 12 months. Most patients report an increase in mobility. In the Coolief clinical study, they found the treatment was longer-lasting and gave greater pain relief than the steroid injections. However, there are risks to all medical procedures discussing your options with your doctor is very important.
Also Check: Stiff Painful Knees After Sitting
How To Avoid Over
Your parent needs to be meticulous in following all the steps of the process with Medicare, so that they get the best coverage for their equipment.
To avoid paying any extra for their DME your parent must use a Medicare enrolled participating supplier who accepts assignment.
This ensures the DME is being bought for the Medicare-approved price, which is as low as it gets, and their co-payment will be as low as is possible as a result.
- Medicare Participating Suppliers
Medicare and Medicare Participating Suppliers have an agreement that Medicare Participating Suppliers will accept what is called assignment this means that they will only charge the Medicare-approved price for DME.
Suppliers who are not Participating can charge up to 15% more for the DME, and as Medicare will only pay the supplier their Medicare-approved price, it leaves your parent to pay the difference, as well as their co-payment and deductible .
Does Medicare Cover Walking Boots
If you were looking for an ice/cold therapy machine because of an injury, or surgery, to your ankle/foot, you may be in luck, because along with walkers, rollators and crutches, Medicare will also cover ankle braces, or orthotics commonly known as walking boots and that can be for both custom-fitted, and off-the-shelf models.
If the walking boots are being used to immobilize the ankle/foot following orthopedic surgery, or for an orthopedic condition, you are eligible for Medicare coverage under the Brace benefit in Medicare Part B.
As long as you have a prescription from a Medicare-enrolled physician which states that it is medically necessary, you will typically be covered.
Also Check: Regrow Cartilage Naturally
Medicare Coverage For Parts A And B
At present, Original Medicare Parts A and B pay for certain costs of knee replacement surgery provided the procedure is deemed medically necessary by the doctor. Part A would cover the expense of the hospital stay while Part B would cover out-patient and recovery services mandated by the physician.
Patients would have to pay Part B deductible and 20% of the co-insurance fees.
Medicare Part C would provide the same coverage as Medicare Part A and B and additional coverage for certain services. If you anticipate knee replacement surgery in the future, can explore Part C plans for better coverage.
Antibiotics, anticoagulants, and painkillers prescribed by the doctor following knee surgery would be covered by Medicare Part Ds prescription drug program or Medicare Advantage Prescription Drug policy.
Patients should check the costs of the procedure and the extensive aftercare that involves pain medications and physical therapy.
Does Medicare Cover Knee Replacement Surgery Costs
If your doctor recommends knee replacement surgery, your first question is probably, how much does a knee replacement cost? Knee surgery cost depends on a number of factors, including where you live, where you have the surgery, whether you have any complications, and the type of care youll need after surgery.
Fortunately, if you have Medicare, the actual knee replacement cost you pay out-of-pocket is limited by rules governing Medicare Part A and Part B. Read on to learn more details about knee replacement cost under Medicare.
Also Check: Copper Care Knee Brace Reviews
She Was A Victim Of The Medicare 3
The 3-day rule is Medicares requirement that a patient has to be admitted to the hospital for at least 3 days in order for Medicare to cover the cost of a SNF after the hospitalization. If the patient is admitted for less than 3 days, then the patient pays the cost of the SNF and Medicare pays nothing. So, if this patient was in the hospital for 4 days, why didnt Medicare cover the cost of the SNF?
It all has to do with when the inpatient stay clock starts and that has nothing to do with when the patient first comes into the hospital for a surgery or a medical condition. It solely depends on when the attending physician entered an order for that patient to be in inpatient status as opposed to observation status. Medicare considers a patient to be in inpatient status if that patient is anticipated to need to be in the hospital for 2 midnights and in observation status if the patient is anticipated to be in the hospital for less than 2 midnights. Observation status was originally intended to be used to observe the patient to determine whether the patient is sick enough to warrant being admitted to the hospital.
American Hospital Association Disclaimer
The American Hospital Association has not reviewed, and is not responsible for, the completeness or accuracy of any information contained in this material, nor was the AHA or any of its affiliates, involved in the preparation of this material, or the analysis of information provided in the material. The views and/or positions presented in the material do not necessarily represent the views of the AHA. CMS and its products and services are not endorsed by the AHA or any of its affiliates.
Also Check: What Do You Do For Water On The Knee
Do Medicare Supplement Plans Cover Knee Replacement Costs
Medicare Supplement plans may help pay for coinsurance, copayments, and possibly deductibles from Medicare Part A and Part B. Different standardized Medicare Supplement plans may cover different services. Find out more about what Medicare Supplement plans might cover.
When youre adding up your Medicare prices, remember that if youre enrolled in a Medicare Advantage plan, you still have to pay your monthly Medicare Part B premium. You also need to pay the Medicare Advantage plan premium whatever that amount may be. Some plans charge as little as $0 a month.
Do you have questions about Medicare coverage options? You can call eHealth to speak with a licensed insurance agent. Use the Browse Plans button on this page to explore Medicare plan options in your area.
The product and service descriptions, if any, provided on these eHealth web pages are not intended to constitute offers to sell or solicitations in connection with any product or service. All products are not available in all areas and are subject to applicable laws, rules, and regulations.
Medicare information is everywhere. What is hard is knowing which information to trust. Because eHealths Medicare related content is compliant with CMS regulations, you can rest assured youre getting accurate information so you can make the right decisions for your coverage. Read more to learn about our Compliance Program.
List Of Durable Medical Equipment Covered By Medicare
If you dont find the equipment you are looking for in my list of Medicare covered DMEs below, you can use this link to Mediace.gov
Air-Fluidized BedAlternating Pressure Pads and MattressesAudible/visible Signal Pacemaker MonitorPressure reducing beds, mattresses, and mattress overlays used to prevent bed soresBead BedBed Side RailsBed Trapeze covered if your loved one is confined to their bed and needs one to change positionBlood sugar monitorsBlood sugar test stripsCanes Commode chairsContinuous passive motion machinesContinuous Positive Pressure Airway Devices, Accessories and TherapyCrutchesVentilators WalkersWhirlpool Bath Equipment if your loved one is homebound and the pool is medically needed. If your loved one isnt homebound Medicare will cover the cost of treatments in a hospital.
Read Also: Tommie Copper Knee Sleeves For Arthritis
How Do You Proceed Once Your Parent Has A Doctors Signed Prescription For A Dme
As long as Medicare Part B is satisfied that your parents DME is medically necessary, they will cover 80% of theMedicare-approved price for the DME.
Your parent will then be responsible for paying their Medicare 20% co-payment of the Medicare-approved price of the DME, as long as they have used a Medicare-enrolled participating supplier who accepts assignment.
If not, your parent may owe much more !
Your parent will also have to pay their deductible, if it hasnt already been met.