Are There Any Complications
Osteoarthritis can develop over just a year or two, but more often its a slow process over many years that only causes fairly small changes in just part of the knee.
But in some cases, the cartilage can become so thin that it no longer covers the ends of the bones. This causes them to rub against each other and eventually wear away.
The loss of cartilage, the wearing of the bones, and the bony spurs can change the shape of the joint. This forces the bones out of their normal positions, making your knee feel unstable and painful.
Some people with osteoarthritis find a lump appears at the back of their knee. This is called a Bakers cyst or popliteal cyst.
A Bakers cyst is fluid-filled swelling at the back of the knee that happens when part of the joint lining bulges through a small tear in the joint capsule. This can then cause joint fluid to be trapped in the bulge.
It can happen on its own, but is more likely in a knee thats already affected by arthritis. A Bakers cyst doesnt always cause pain, but sometimes they can burst so the fluid leaks down into your calf, causing sharp pain, swelling and redness in the calf.
Osteoarthritis in the knee might change the way you walk or carry your weight, and this could cause you to develop the condition in other joints, such as your hips.
How Is Oa Treated
There is no cure for OA, so doctors usually treat OA symptoms with a combination of therapies, which may include the following:
- Increasing physical activity
- Medications, including over-the-counter pain relievers and prescription drugs
- Supportive devices such as crutches or canes
In addition to these treatments, people can gain confidence in managing their OA with self-management strategies. These strategies help reduce pain and disability so people with osteoarthritis can pursue the activities that are important to them. These five simple and effective arthritis management strategies can help.
Physical Activity for Arthritis
Some people are concerned that physical activity will make their arthritis worse, but joint-friendly physical activity can actually improve arthritis pain, function, and quality of life.
Osteoarthritis Of The Knee
Knee OA is a very common source of pain that can limit your mobility.
Causes of Knee OA
The cause of OA is unknown. These risk factors make it more likely you will develop knee OA:
- Age: OA can occur at any time of life, but it is most common in older adults.
- Sex: Women are more likely to have knee OA than men.
- Obesity: Being overweight adds stress to your knees. Fat cells also make proteins that can cause inflammation in and around your joints.
- Injuries: Any knee injury, even old ones, can lead to knee OA.
- Repeated stress: Frequent stress on your knee from your job or playing sports can increase risk for OA.
- Genetics: You can inherit a tendency to develop OA.
- Bone deformities: If you have crooked bones or joints, you are at higher risk.
- Some metabolic diseases: Diabetes and hemochromatosis, a condition in which your blood has too much iron, have been linked to OA
Symptoms of knee OA develop slowly and worsen over time.
- Pain: Movement causes pain. Sometimes your knee will ache while sitting still.
- Stiffness: Your knees may be stiff first thing in the morning or after sitting for a long time.
- Loss of motion: Over time, you may lose the ability to bend and straighten your knee all the way.
- Creaking and grating : You may hear crackling noises or feel a grating sensation.
- Instability: Your knee may give out or buckle, or feel like it could.
- Locking: The knee may lock or stick.
- Swelling: Your knee may get puffy all around or on one side.
Your doctor will check for:
Also Check: Is Second Knee Replacement Easier
How Is Hip Osteoarthritis Diagnosed
Doctors can use several different tests to diagnose joint disease. Usually the first test performed is an x-ray. X-rays are taken of the hip and the surrounding bones and then carefully examined. Bone spurs are a common indicator of arthritis, and the narrowing of the joint itself can usually be seen in the x-ray as well. If this is not conclusive, most doctors will send the patient to get an MRI of the hip area. This test is generally to find out the extent of the degeneration and to help the doctor get the best idea of the condition of the patient. Some doctors will also order blood work to rule out other diagnoses, and in some cases they may draw fluid from the hip joint to examine it. Once a diagnosis has been made, a treatment plan can begin.
What Are The Symptoms Of Degenerative Joint Disease In The Knee
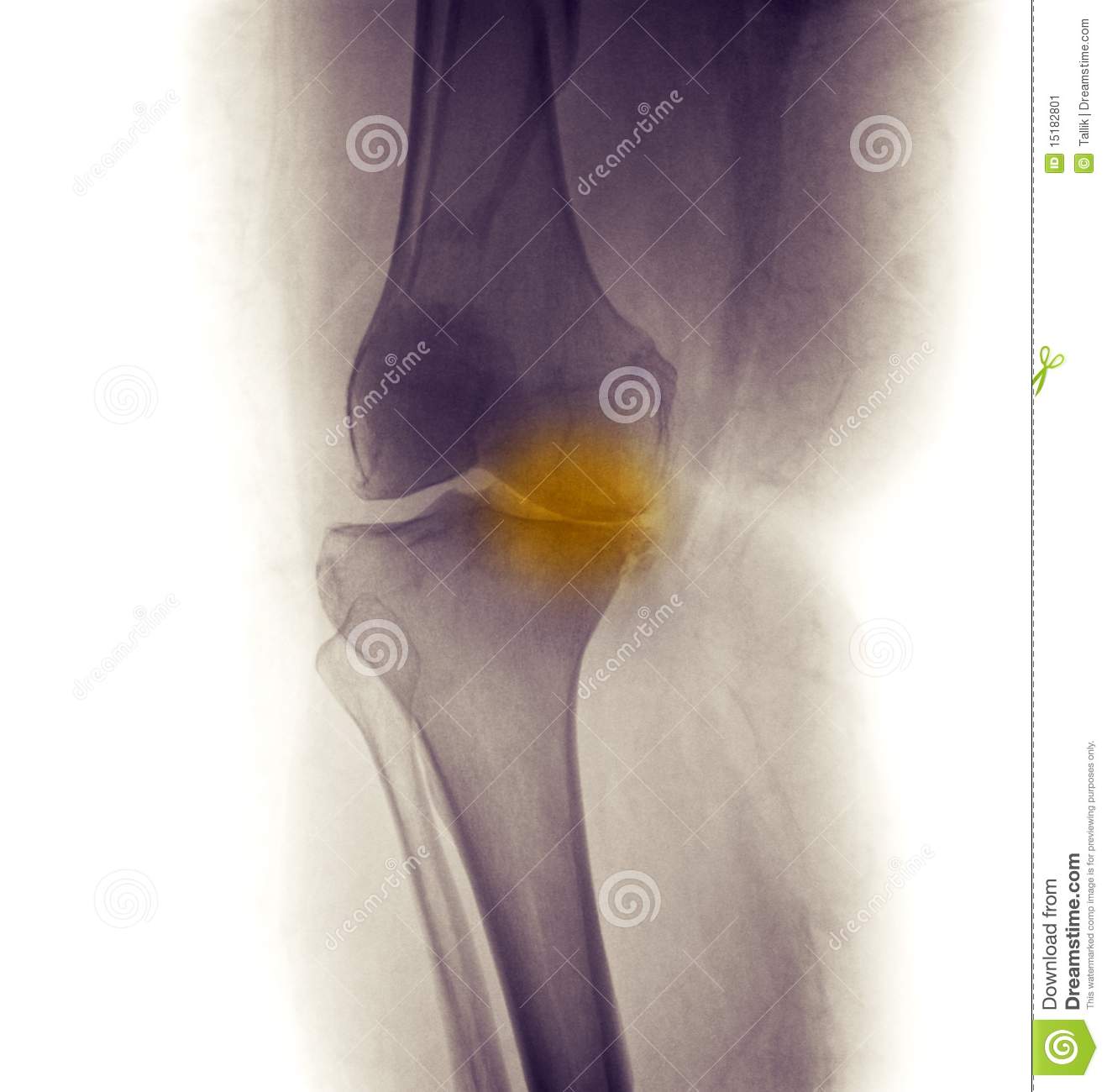
The most common symptom of knee arthritis is persistent knee pain. Typically, the knee pain gets worse over time and is worse right after getting up in the morning or after sitting for a while. Other common symptoms include
- Stiffness in the knee
- Grinding or clicking sound in the knee
- Feeling of instability or catching in the knee
If youre experiencing any of these symptoms, it may be time to seek an orthopaedic evaluation for degenerative joint disease.
Don’t Miss: How To Help With Knee Pain After Running
How Is Knee Arthritis Diagnosed
Your doctor may use some of the following diagnostic tests and procedures to determine if you have knee arthritis:
- Medical history and physical examination
- Blood tests for genetic markers or RA antibodies
- X-rays to determine cartilage loss in the knee
- Joint aspiration: drawing out and testing the synovial fluid inside the knee joint
Cartilage cannot be seen on X-ray, but narrowing of the joint space between the bones indicates lost cartilage. X-rays show bone spurs and cysts, which can be caused by osteoarthritis. Other tests such as MRI or CT scans are rarely needed for diagnosis.
Natural Degenerative Joint Disease/osteoarthritis Treatment
While it might not be possible to totally cure degenerative joint disease once its developed, there are a lot of natural osteoarthritis treatment options available that can make a big impact. These include: exercising and staying active, preventing weight gain and maintaining a healthy body weight, eating an anti-inflammatory diet, and treating pain using physical therapy, sauna treatments, massage therapy and essential oils. All of these help lower severity of symptoms and slow progression of the disease so more cartilage is spared.
The primary goals of all degenerative tissue disease/osteoarthritis or arthritis treatments are to lower inflammation/swelling, control pain, improve mobility and joint function, help maintain a healthy weight so you put less pressure on fragile joints, and to improve your mood so youre better able to handle the stress of battling a degenerative disease.
1. Stay Active
While most people with osteoarthritis usually have joint pain and some movement limitations, many find that they feel better and experience less symptoms overall when they keep moving. In fact, exercise is considered one of the most important treatments for degenerative joint disease. Like the old saying goes, Move it or lose it. In other words, the more you strengthen and stretch your body parts, the better intact theyll stay into older age.
2. Lower Inflammation and Support Cartilage with a Nutrient-Dense Diet
Focus your diet around these foods as much as possible:
Don’t Miss: Does Exercise Help Arthritic Knees
Conservative Degenerative Joint Disease Treatments
If you have developed moderate degenerative joint disease, the following treatments may be helpful in easing your pain and discomfort:
- Pain medications
- Epidural steroid injections
However, if you do not experience adequate relief from your symptoms after several weeks or months, USA Spine Cares minimally invasive spine surgery may be able to help you on the road to recovery.
Djd Vs Rheumatoid Arthritis
Rheumatoid arthritis is not the same as DJD. Rheumatoid arthritis is an autoimmune disorder rather than a degenerative condition that can be caused by natural wear and tear. While they share similar symptoms, they are nevertheless different conditions and require different treatment methods to manage.
Read Also: How To Slow Down Arthritis In Knees
When Should I Consider Surgery
When the conservative measures above are not enough and pain in a specific joint makes it difficult for you to move, then can restore your comfort and help you to return to normal activity. surgery and surgery have become trusted treatments for restoring mobility and easing pain.
For cases of hip and knee arthritis, some patients may be able to have less invasive hip arthroscopy or knee arthroscopy procedures. Joint replacement surgery may also be an option for people with arthritis of the, , wrist or .
You are generally a good candidate for surgery if conservative treatment hasn’t worked and you experience a significant interruption in some activity of daily life for example, if you can’t walk more than a city block or if you awaken from sleep with pain in the affected joint. In such cases, surgery should provide outstanding results, because you will become pain-free in the affected joint. The exact type of surgery you have will depend on your age, activity level, and the specific joint that is affected.
How Will It Affect Me
If you have osteoarthritis of the knee, you will probably feel your knee is painful and stiff at times. It may only affect one knee, especially if youve injured it in the past, or you could have it in both. The pain may feel worse at the end of the day, or when you move your knee, and it may improve when you rest. You might have some stiffness in the morning, but this wont usually last more than half an hour.
The pain can be felt all around your knee, or just in a certain place such as the front and sides. It might feel worse after moving your knee in a particular way, such as going up or down stairs.
Sometimes, people have pain that wakes them up in the night. Youll probably find that the pain varies and that you have good and bad days.
You might find you cant move your knee as easily or as far as normal, or it might creak or crunch as you move it.
Sometimes your knee might look swollen. This can be caused by two things:
- Hard swelling: when the bone at the edge of the joint grows outwards, forming bony spurs, called osteophytes .
- Soft swelling: when your joint becomes inflamed and produces extra fluid, sometimes called an effusion or water on the knee.
Sometimes osteoarthritis of the knee can cause the muscles in the thighs to weaken, so your leg may look thinner. This weakness can make the joint feel unstable and could cause the knee to give way when you put weight on it.
Don’t Miss: Why Does My Knee Click
What Is The Prognosis Of Degenerative Joint Disease
Prognosis of DJD can vary, with some patients unaffected by the condition and others who become severely disabled. For many people, joint replacement surgery offers the best long-term outcome for DJD.
As the population ages, the number of people with osteoarthritis will grow. It is estimated that by 2030, 20 percent of Americans about 72 million people will have passed their 65th birthday and will be at high risk for the disease. If you believe you have symptoms od DJD, we can help. Call the Florida Spine Institute for an appointment.
The Damage And Loss Of Knee Cartilage
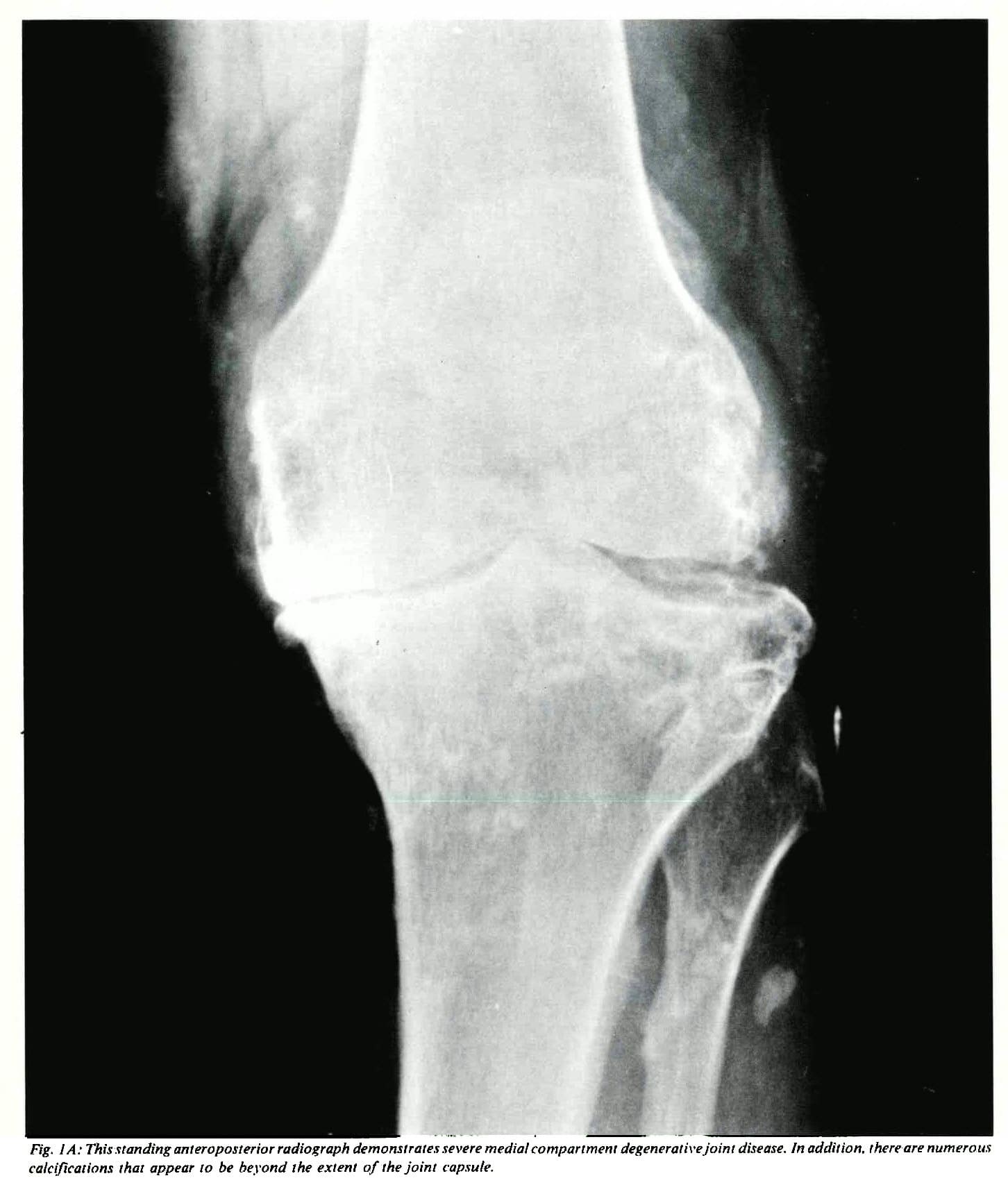
The defining feature of osteoarthritis is the breakdown and loss of articular cartilage. In the knee, articular cartilage covers the top of the tibia , the bottom of the femur and the back of the patella . Articular cartilage protects the surfaces of these bones where they meet at the joint. During the development of osteoarthritis:
- Cartilage weakens. The composition of the articular cartilage changes, becoming weaker. This change in composition is especially common in older age.
- Cartilage becomes damaged. The weakened articular cartilage thins or wears away.
- Cartilage may attempt to heal. The damaged cartilage may attempt to produce new cells, but it is not enough to replace the missing cartilage. In addition, these new cells may grow in irregular, bumpy patterns rather than the smooth pattern of the original cartilage.
- Meniscus damage is likely. Damage to the knees meniscus is likely to also occur.1Englund M, Guermazi A, Lohmander LS. The meniscus in knee osteoarthritis. Rheum Dis Clin North Am. 2009 Aug 35:579-90. doi: 10.1016/j.rdc.2009.08.004. Review. PubMed PMID: 19931804. Because meniscal cartilage is different from articular cartilage, meniscus damage is considered a separate but related condition to knee osteoarthritis.
Don’t Miss: Where To Buy Donjoy Knee Braces
Is There Anything I Can Do To Prevent Djd
Many dogs with from DJD are overweight. If your dog is overweight, it is imperative that he or she loses weight in a controlled manner. Low or restricted calorie diets are helpful in preventing excessive weight gain and for losing weight. There are many weight-reducing diets available that work very well for most dogs. Your veterinarian can help you design an appropriate weight loss program for your pet .
Citation Doi & Article Data
Citation:DOI:Henry KnipeRevisions:see full revision historySystem:
- Early osteoarthritis of the knee
- Degenerative disease of the knee
- Knee osteoarthritis
- Degenerative joint disease of the knee
Osteoarthritis of the knee is very common and is a major cause of morbidity, especially in the older population.
Recommended Reading: When To Get Knee Surgery
Key Takeaways For Degenerative Joint Disease:
- Degenerative joint disease, also called osteoarthritis, is the leading type of arthritis in adults.
- DJD results in decreased cartilage and joint tissue, which leads to joint pain, inflammation and trouble moving.
- Its caused by a combination of factors: genetics, high inflammation, poor diet, inactivity, repetitive motions and getting older .
- You can help prevent and treat degenerative joint disease naturally by eating a nutrient-dense diet, staying active, reducing stress, and relieving pain with alternative treatments like acupuncture, massage therapy and heat/cold applications.
How Is Degenerative Joint Disease Treated
Getting a medical opinion at the right time can help arrest the progress of the disease even though it can not be completely reversed. The treatment of osteoarthritis is based on the symptoms and the locations where they are experienced. Doctors treat this condition with a combination of therapies including: rest, lifestyle changes, dietary changes, exercise, weight loss, hot/cold therapy, as well as over-the-counter medication such as oral and topical analgesics.
Additionally, nonsteroidal anti-inflammatory drugs, acetaminophen, or even corticosteroids orally or as an injection may be recommended to produce the best results in terms of reduction of symptoms.
The process of viscosupplementation has also become common of late as it reduces the pain in the joints. A gel-like substance that is similar to the natural lubricant in the joints is injected into the region to create the cushioning effect that Osteoarthritis removes from the joints.
Often, physical and occupational therapists may be involved by your physician to assist you in the process of rehabilitation via a combination of therapies and exercises. In case none of these treatments have proved their efficacy, your physician may recommend that you consult a spinal surgeon or orthopedic surgery for surgical processes known as arthroplasty and total joint arthroplasty.
What are treatments offered by Advanced Pain Care for degenerative joint disease?
You May Like: What To Expect After Full Knee Replacement
Do I Need Additional Examinations
- Diagnostic examination for other non-physical factors important for your pain, have already been done by yourself trough filling out your pain questionnaires.
- Blood tests are required when systemic conditions such as arthritis are suspected.
- If the knee problems continue to persist: X-rays and an MRI scan.
Radiographic Findings Of Oa
- Joint space narrowing
- Advice on weight loss
- The first-line treatment for all patients with symptomatic knee osteoarthritis includes patient education and physiotherapy. A combination of supervised exercises and a home exercise program have been shown to have the best results. These benefits are lost after 6 months if the exercises are stopped.
- Weight loss is valuable in all stages of knee OA. It is indicated in patients with symptomatic OA with a body mass index greater than 25. The best recommendation to achieve weight loss is with diet control and low-impact aerobic exercise.
- Knee bracing in OA can be used. Offloading-type braces which shift the load away from the involved knee compartment. This can be effective when there is a valgus or varus deformity.
Other non-physiotherapy based interventions include pharmacological management:
You May Like: How To Get Rid Of Crepey Skin On Knees
Professional Treatment And Care
It is important that patients with symptoms of hip osteoarthritis contact a doctor as soon as possible. Many painful symptoms can be treated with the right care. Early care can prevent more serious symptoms appearing and help the patient regain mobility and health. There is no cure for joint disease, but there are many things that can be done to help the patient live a happy and healthy life with minimal pain.
What Is Advanced Djd
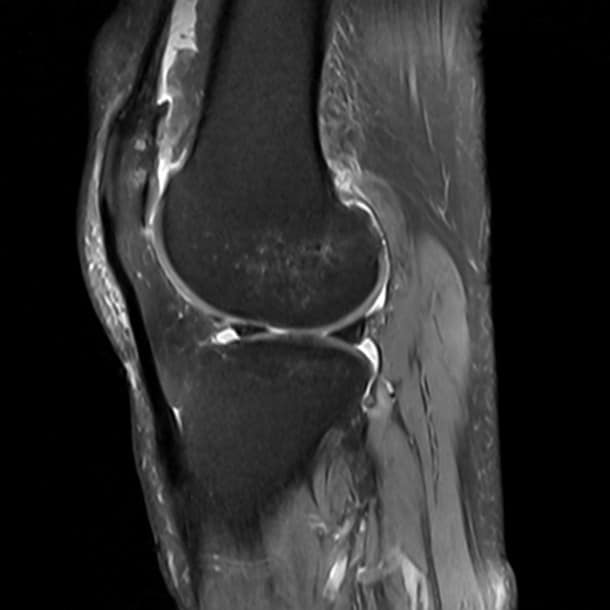
Advanced DJD of the knee is the breakdown of the cartilage and instability of the knee which causes pain, swelling, loss of motion and activity. In knee osteoarthritis the cartilage protecting the bones of the knee slowly wears away. Your knee is divided into three major compartments: the medial compartment, the inside of the knee the lateral compartment, the outside of the knee and the patellofemoral compartment, the front of the knee between the knee cap and thighbone.
Advanced osteoarthritis in the knee can be limited to a one, two or all three compartments . Unicondylar knee arthroplasty can replace the medial compartment, leaving the remaining joint surfaces intact. A patellofemoral joint arthroplasty can replace the surfaces on the back of the kneecap. These are more conservative that a total joint replacement and allow for a quicker recovery. In cases of two or three compartment DJD, a total knee arthroplasty is indicated. This is one of the most common orthopedic procedures performed in the world.
Recommended Reading: How To Relieve Knee Joint Pain