Are Any Tests Needed To Diagnose Chondromalacia Patellae
Often, no tests are needed, as treatment can be started on the basis of a working diagnosis of chondromalacia.
Tests may be used in some situations, either to confirm the diagnosis or to rule out other causes. For example, if the diagnosis is not clear, or if symptoms do not improve after treatment. Tests which may be used are:
- Blood tests and/or a standard knee X-ray – these may help to rule out some types of arthritis or inflammation.
- Arthroscopy – a tiny flexible camera is inserted into the knee to see exactly what the cartilage looks like. This requires an anaesthetic and has a small risk of complications.
How Is Chondromalacia Patellae Diagnosed
Usually, a provisional diagnosis of chondromalacia patellae is made from your symptoms plus a doctor’s examination of the knee. This will be a working diagnosis rather than a definite one, because the cartilage cannot be seen without further tests . In this situation, where there is no proof of chondromalacia, some doctors call the pain patellofemoral pain syndrome or anterior knee pain. This does not matter, as the treatment will be the same at this point .
What Is The Orthopaedic Test For Chondromalacia Patella
Having a patient relax with their knee out straight and then moving the kneecap in the end of the femur is a good way to assess for any crunching or pain with moving of the patella. In some cases, the patients may also have some chondromalacia of the opposing surface of the femur and it may not be definitive as to whether the chondromalacia is at the patella or the femur. In addition, having a patient stand up and lunge or squat to the point where they hurt can also be definitive as to the presence of chondromalacia being symptomatic when one does feel this crepitation with moving the patella in the trochlear groove.
Also Check: Nano Knee Surgery Cost
Treatment For Chondromalacia Patellae
Treatment for knee chondromalacia will depend upon the extent of the damage, as determined by chondromalacia grading. A chondromalacia patella MRI can be used to evaluate the damage.
For mild chondromalacia, treating the condition with a period of rest from aggravating activities along with the application of ice and compression along with anti-inflammatory medications can be very effective. If the cause is a mistracking patella, applying tape or wearing a chondromalacia knee brace can help relieve the symptoms of chondromalacia.
Once the swelling is under control, one will likely need to undergo physical therapy and cross-training to improve ones strength and flexibility. At this point, a patella tracking brace may also be helpful. (Check out an article on The Benefits of Knee Braces for Rehabilitation.
But if these initial lines of defense are not helpful for relieving chondromalacia pain, surgery to remove the damaged cartilage may be necessary. BraceAbility also offers a number of post-operation knee braces for immediately following the surgery.
View all of BraceAbility’s knee injury treatments, including specific treatment options for chondromalacia.
Diagnosing And Grading Chondromalacia Patellae
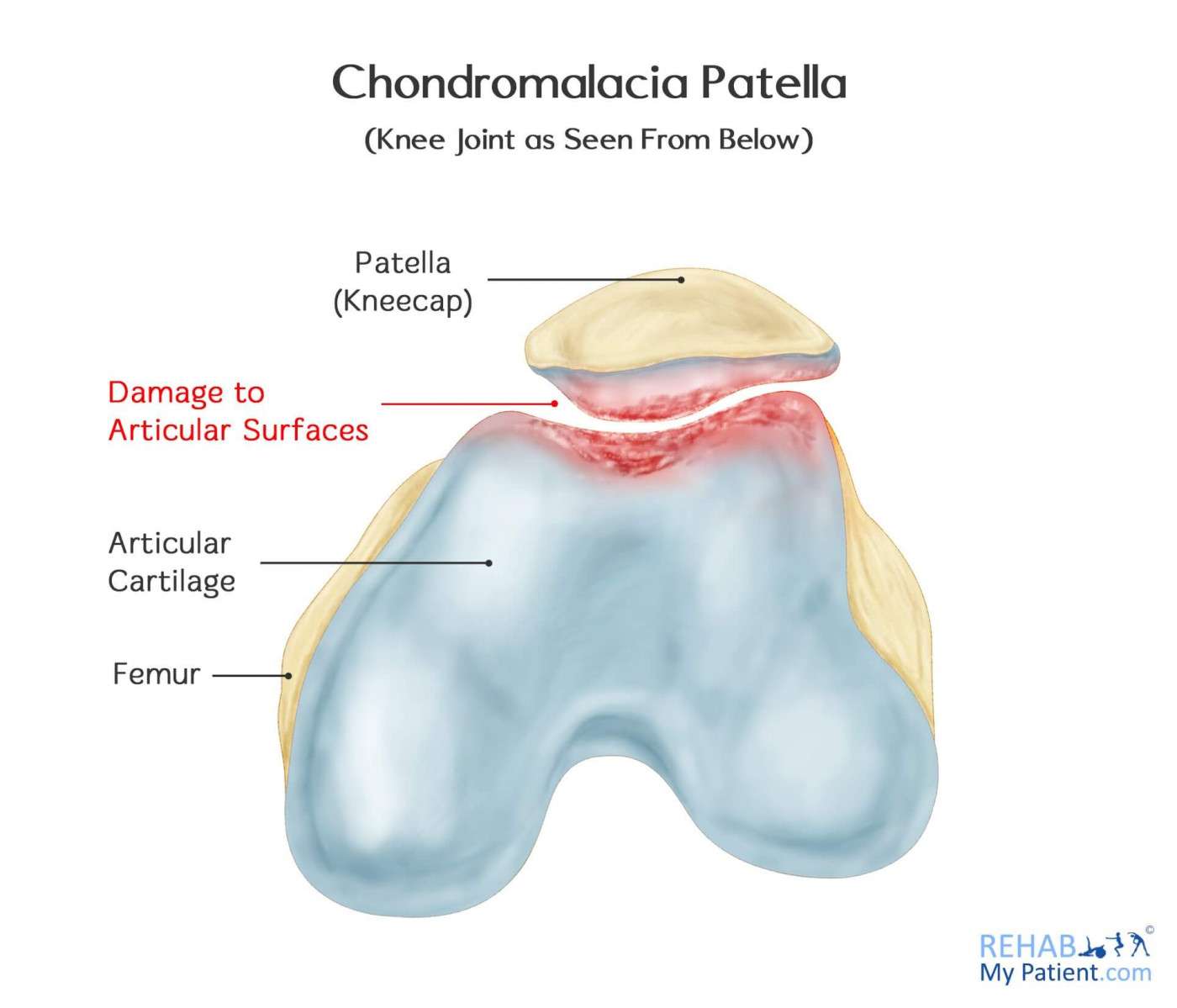
Your doctor will look for areas of swelling or tenderness in your knee. They may also look at how your kneecap aligns with your thigh bone. A misalignment can be an indicator of chondromalacia patellae. Your doctor may also apply resistive pressure to your extended kneecap to determine the tenderness and severity.
Afterward, your doctor may request any of the following tests to aid in diagnosis and grading:
- X-rays to show bone damage or signs of misalignment or arthritis
- magnetic resonance imaging to view cartilage wear and tear
- arthroscopic exam, a minimally invasive procedure to visualize the inside of the knee that involves inserting an endoscope and camera into the knee joint
Don’t Miss: How Much Does Aflac Pay For Ambulance Ride
Diagnosing And Grading Chondromalacia Patella
The main symptoms of chondromalacia are unfortunately common to many disorders of the knee. So the only way to truly be sure of a diagnosis of chondromalacia is by getting an MRI, which allows us to see the cartilage inside the knee. As an orthopedic surgeon, my biggest concern is not just whether you have chondromalacia, but what has caused it. When I do an exam as a doctor, I will be looking for flat feet, abnormal knee alignment, or other causes of chondromalacia that can be corrected.
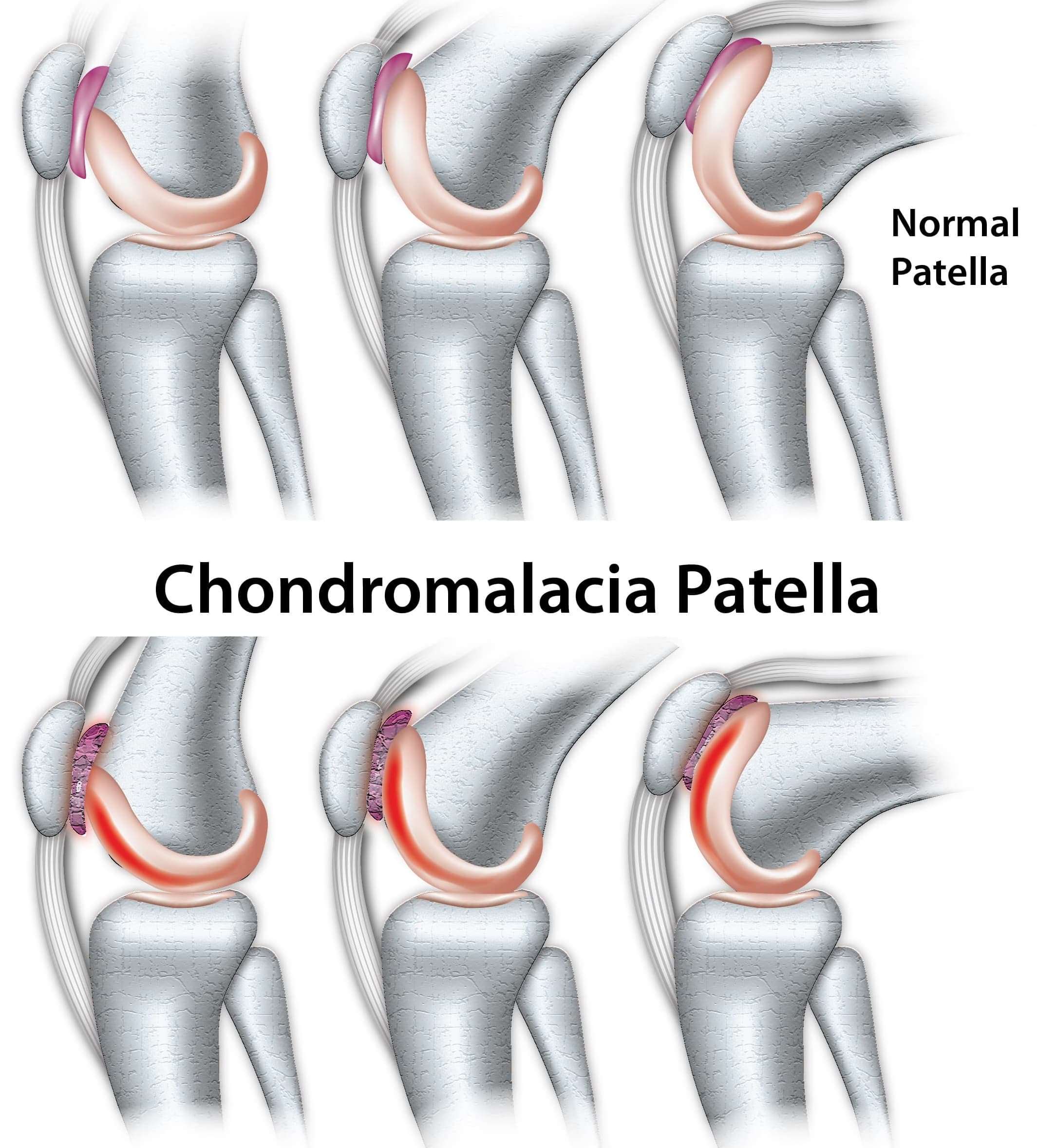
Orthopedic surgeons grade chondromalacia on a scale of 1 to 4.
- Grade 1 chondromalacia is merely softening of the cartilage.
- Grade 2 is when the cartilage surface begins to break up, and the cartilage becomes rough.
- Grade 3 is when long fissures develop in the cartilage, often with loose flaps of cartilage. Grade 3 may also show partial thickness loss of the cartilage.
- Grade 4 chondromalacia is when the cartilage peels off or wears down to the bone underneath.
Does Chondromalacia Patella Lead To Patellar Tilt
Many cases of patella chondromalacia involve a wearing away of the cartilage on the outside part of the kneecap joint. Therefore on x-ray, it can appear that the patella is tilting because the cartilage space is less than it should be normally. In these cases, the patella is not truly tilting and the regular treatment for patellar chondromalacia should be followed. A lateral release in this indication would have little chance of benefiting these symptoms.
You May Like: How Do I Get Rid Of Fat Around My Knees
Does Chondromalacia Patella Show Up On An Mri
The diagnosis of chondromalacia patella on MRI can be definitive, but it can be directly correlated to the strength of the magnet for the MRI. Low-field strength MRIs, such as those with 1.0 or 1.5 Tesla magnets, may not show chondromalacia as well as higher-field strength Tesla magnets such as a 3.0 Tesla MRI scan. In addition, patients who have swelling of their knee can often have the MRI more definitively show the area of chondromalacia because fluid can leak into the crevices and cracks that are present with the chondromalacia patella.
What Are The Types Of Knee Replacement Surgery
There are two types of knee replacement surgeries. They are referred to as partial and full knee replacement.
In a partial knee replacement, the surgeon removes a part of the damaged knee joint. They will then replace the damaged knee joint with a metal or plastic prosthesis.
In a full knee replacement, the surgeon removes the damaged knee joint. They will replace the damaged knee joint with a metal or plastic prosthetic.
Don’t Miss: Nano Knee Cost
Surgical Treatments For Chondromalacia
An arthroscopy is the most common type of surgery performed for chondromalacia.
Your physician may recommend arthroscopy to check the cartilage around your kneecap. If the cartilage is softened or shredded, the surgeon will remove those layers during the surgery.
If re-alignment of your kneecap, or other parts of the knee, to reduce the wear and tear on your knee cartilage is necessary, this may also be done during surgery.
Is Obesity Associated With Patellar Chondromalacia
In patients who are overweight or obese, when they squat, lunge or generally put extra stress on the front of their knee, they can exacerbate or cause chondromalacia patella. Therefore, losing weight can be a good way to decrease some of the symptoms with chondromalacia patella because it will decrease the forces over the front of the knee and potentially lead to a slowing down of the breakdown of the cartilage surface.
Recommended Reading: Inversion Table After Hip Replacement
Treatment Options For Chondromalacia Patellae
The goal of treatment is to reduce the pressure on your kneecap and joint. Resting, stabilizing, and icing the joint may be the first line of treatment. The cartilage damage resulting in runners knee can often repair itself with rest.
Your doctor may prescribe several weeks of anti-inflammatory medication, such as ibuprofen, to reduce inflammation around the joint. If swelling, tenderness, and pain persist, the following treatment options may be explored.
Chondromalacia Patella Recovery Time
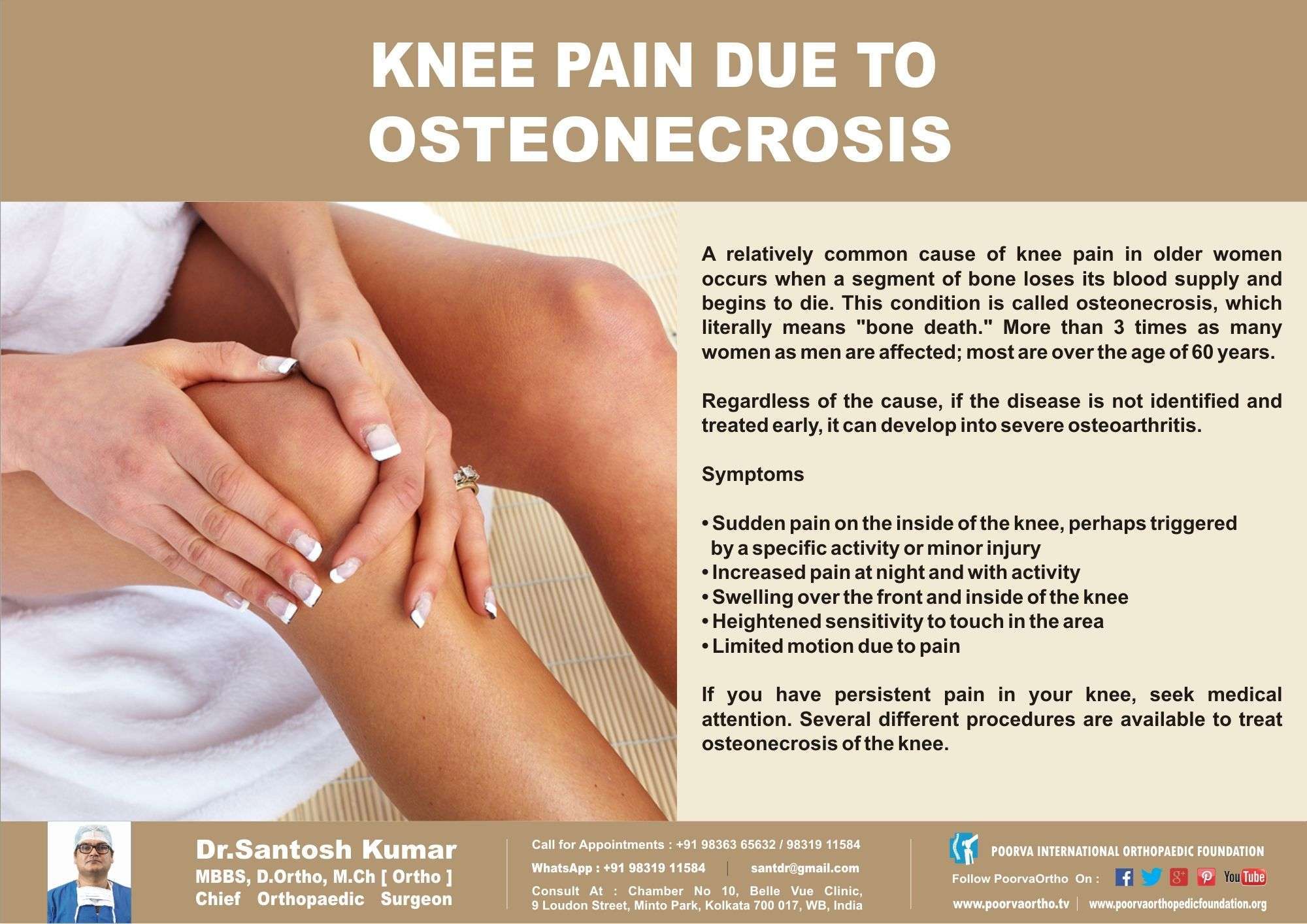
The time required for a full recovery from chondromalacia patella varies based on a number of factors, including the grade of the condition, your lifestyle, and treatments used. However, most cases heal within weeks or months with the use of minimally invasive treatments. The top treatment option is physical therapy for restoring better knee alignment. Other options for managing pain include acupuncture, chiropractic care, and massage therapy.
Similarly, arthroscopic knee surgery recovery time varies depending on circumstances. After chondromalacia surgery, you may need to use a brace and ice pack to alleviate pain, and physical therapy should begin within days.
For the best chance of a quick recovery, address your symptoms immediately and always focus on good form with daily activities. Consult your doctor and use the RICE protocol without delay to help manage pain and swelling effectively.
Recommended Reading: Bioknee Cost
Why Do We Have Kneecaps
The patella is a small, triangular shaped bone that sits inside the quads muscles at the front of the thigh.
It rests in a special dip know as the patella groove on the front of the thigh bone, the femur, where it moves up and down as you move your leg.
The patella is lined with the thickest cartilage in the whole body which:
- Ensures the patella glides smoothly over the knee bones
- Works as a shock absorber
Not only does the patella help to protect the knee joint, it also helps the quads muscles work more effectively, by reducing the amount of force needed to move the knee.
What Type Of Rehabilitation Program Should Be Followed For Chondromalacia Patella
In general, one should follow a rehabilitation program which does not exacerbate the underlying symptoms and also works on lower-impact strengthening for that affected knee. These exercises include the use of a stationary bike, pool therapy to include swimming, the use of an elliptical machine, and walking. Working on strengthening ones hips has also been found to be beneficial for helping anterior knee pain. In general, lunges, squats, and knee extension exercises on machines at the gym can exacerbate underlying chondromalacia symptoms.
Also Check: Knees Crack When Doing Squats
Can Chondromalacia Be Cured
At this time the answer is no. We do know that our diet and exercise influence the health of our cartilage. Therefore it is important to avoid ultra-processed foods and eat a diet of real food with plenty of fruits and vegetables too. Exercise can help your body to repair itself. It turns on the production of your internal anti-inflammatories, and it helps the cartilage strengthen itself. The pain from chondromalacia can often be treated. Common treatments for chondromalacia include:
- Physical therapy
- Compression sleeves- used to try and decrease pain while you start an exercise program
- injections
Most patients can lead very active lives after treatment is started. You do need to commit to an exercise program for a while. You might not start to see improvement for 2-3 months. There is ongoing very active research into medications that appear to show promise in reversing or halting the progress of chondromalacia or arthritis. Wnt inhibitors are medications that may be available over the next 3-7 years. Early data shows that Wnt inhibitors might eventually be able to reduce or cure arthritis. Very exciting recent development.
What Are The Surgical Treatment Options For Chondromalacia
If nonsurgical treatments are not successful, or if you have severe symptoms, your doctor may recommend knee arthroscopy. Arthroscopy is a minimally invasive operation in which the surgeon examines the joint with an arthroscope, a pencil-thin device equipped with a camera lens and light, while making repairs through a small incision. If necessary, your doctor also can correct the alignment of your kneecap or other parts of your knee to help to reduce wear and tear on your knee cartilage.
You May Like: Dcf Compression Knee Sleeve
Nonsurgical Rehabilitation And Treatment
Non-operative treatment is the usual treatment for this problem. You may require 4-6 weeks of physiotherapy treatment, and then several more months of a home stretching and strengthening program to treat your chondromalacia patella. Getting the pain and inflammation under control is the first step. The overall goals for a rehab plan are to provide pain relief or pain control, improve muscle function and flexibility, improve knee alignment, and avoid further wear and tear.
Your physician may suggest anti-inflammatory medications, such as aspirin or ibuprofen, as another means of combating the inflammation and pain. Acetaminophen or paracetamol may be suggested for pain control if you can’t take anti-inflammatory medications for any reason.
Once the initial pain and inflammation has calmed down, your physiotherapist will focus on improving the flexibility, strength, and alignment around the knee joint and entire lower extremity. Static stretches for the muscles and tissues around the knee will be prescribed by your physiotherapist early on in your treatment to improve flexibility. Again, any tightness in the muscles or tissues around the knee can increase the pull on the patella and affect alignment during walking, running or jumping so it is important to address this immediately.
The muscles of the hip that work to align the knee over top of the foot also have a tendency to be weak so specific attention will be paid to them in the rehabilitation process.
Treatment Options For Chondromalacia:
The treatment of chondromalacia will vary depending on how severe it is. Not everyone with softening of the patella cartilage has pain. In cases of mild chondromalacia, with minimal cartilage damage, physical therapy and exercises to strengthen the muscles supporting your kneecap can be very effective. As I mentioned above, the benefits of exercise cannot be over-emphasized. Rest is very rarely the answer for people with anterior knee pain.
In addition to stimulating the production of our bodys own anti-inflammatories like IL-10, other tests such as an MRI have shown that rest can actually lead to cartilage thinning. Exercise can lead to an improvement in cartilage health. When I talk about exercise I am referring to both aerobic and resistance exercises. Walking is a great form of aerobic exercise, but it is not a good form of resistance exercise. Resistance exercise involves bodyweight exercises or some forms of weight training. Working with an athletic trainer or physical therapist is important so that you can learn the proper exercises and their proper form.
A compression sleeve often offers relief to many chondromalacia sufferers. If you are a runner and experience pain in the front of your knee, minimizing hill running, changing your running technique can be effective as well. On occasion, we might inject someone who is very uncomfortable and their knee is swollen and very painful.
Recommended Reading: How Much Does Aflac Pay For Knee Surgery
Which Weightlifting Exercises Should Be Avoided With Chondromalacia Patella
The kneecap joint sees some of the highest forces in the knee. These forces are expressively increased when one is squatting or lunging. Therefore, exercises which involve squatting and lunging can either exacerbate underlying chondromalacia patella or potentially lead to a breakdown of the cartilage surface due to the excessive force and cause chondromalacia patella.
What Are The Treatments For Chondromalacia Patella
Initially, managing pain and inflammation involves
- avoiding motions or activities that irritate cartilage under the kneecap
- ice packs, and
- anti-inflammatory medications can also be helpful in reducing pain and inflammation.
The primary goal for treatment and rehabilitation of chondromalacia patella is to create a straighter pathway for the patella to follow during quadriceps contraction.
- Selective strengthening of the inner portion of the quadriceps muscle will help normalize the tracking of the patella.
- Cardiovascular conditioning can be maintained by stationary bicycling , pool running, or swimming .
- Reviewing any changes in training prior to developing chondromalacia patella pain, as well as examining running shoes for proper biomechanical fit, are critical to avoid repeating the painful cycle. Generally, full-squat exercises with weights are avoided.
- Occasionally, bracing with patellar centering devices is required. Physical therapy can be helpful to begin the strengthening program and to organize optimal exercise routines.
- Stretching and strengthening the quadriceps and hamstring muscle groups is critical for an effective and lasting rehabilitation of chondromalacia patella. “Quad sets” are the foundation of such a program. Quad sets are done by contraction the thigh muscles while the legs are straight and holding the contraction for a count of 10. Sets of 10 contractions are done between 15-20 times per day.
You May Like: Best Knee Walker 2016
What Are The Possible Complications Of A Grade 4 Chondromalacia Knee Replacement
There are no specific complications that are more likely to occur in a patient with a grade 4 chondromalacia knee replacement.
The risk of complications is the same for both the partial knee replacement and the full knee replacement.
What does the recovery of a grade 4 chondromalacia knee replacement look like?
The recovery from a grade 4 chondromalacia knee replacement is the same as any other knee replacement surgery. The patient will have physical therapy to help restore the knee to its normal function.
It will take time to recover completely.
Is Chondromalacia Patella A Disability
A disability rating in excess of 20 percent for chondromalacia patella of the right knee is denied. A separate disability rating of 10 percent for degenerative joint disease with noncompensable limitation of extension of the left knee is granted, subject to the provisions governing the award of monetary benefits.
Also Check: Does Aflac Pay For Sprains
Should One Use A Stationary Bike For Chondromalacia Patella
One of the most beneficial exercises for chondromalacia patella is use of a stationary bike. This is because it is a low-impact exercise which can strengthen the quadriceps and lower extremity muscles to improve ones absorption when one loads their joint. Some patients, although rare, with patellar chondromalacia do have pain with an exercise bike. In these circumstances, these patients should see a physician to determine if an arthroscopy is needed because of the cracks and fissures of their kneecap causing this type of pain.
What Causes Anterior Knee Pain
Activities that require excessive repetitive bending of the knee and occurs more in Over 40s as the cartilage breaks down due to wear and tear. Teenagers particularly girls, where the cartilage softens due to changing pressures on the knee joint due to growth and muscle imbalances at the knee.
What are the Symptoms? General tenderness at the front of the knee that worsens after prolonged sitting, using stairs, standing after sitting and repetitive bending. A grating or grinding sensation may also be felt.
Also Check: My Knees Crack When I Squat