Meniscus Tears Of The Knee
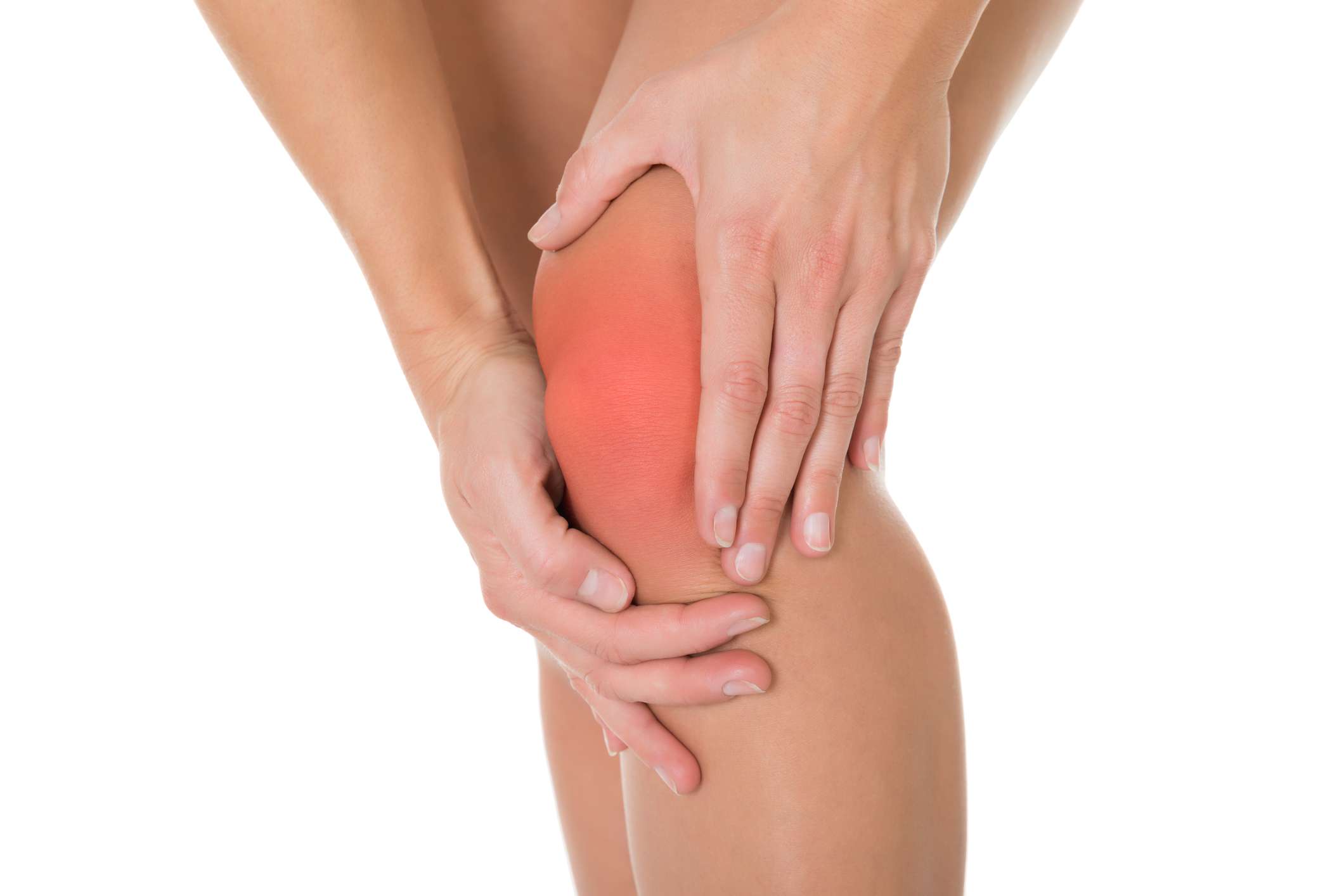
The meniscus can be torn with the shearing forces of rotation that are applied to the knee during sharp, rapid motions. This is especially common in sports requiring reaction body movements. There is a higher incidence with aging and degeneration of the underlying cartilage. More than one tear can be present in an individual meniscus. The patient with a meniscal tear may have a rapid onset of a popping sensation with a certain activity or movement of the knee. Occasionally, it is associated with swelling and warmth in the knee. It is often associated with locking or and unstable sensation in the knee joint. The doctor can perform certain maneuvers while examining the knee which might provide further clues to the presence of a meniscal tear.
Routine X-rays, while they do not reveal a meniscal tear, can be used to exclude other problems of the knee joint. The meniscal tear can be diagnosed in one of three ways: arthroscopy , arthrography, or an MRI. Arthroscopy is a surgical technique by which a small diameter video camera is inserted through tiny incisions on the sides of the knee for the purposes of examining and repairing internal knee joint problems. Tiny instruments can be used during arthroscopy to repair the torn meniscus.
Gradual Increase In Pain
Arthritis pain usually starts slowly, although it can appear suddenly in some cases.
At first, you may notice pain in the morning or after youve been inactive for a while. Your knees may hurt when you climb stairs, stand up from a sitting position, or kneel. It may hurt just to go for a walk.
You may also feel pain when youre simply sitting down. Knee pain that wakes you up from sleep can be a symptom of OA.
For people with RA, the symptoms often start in the smaller joints. They are also more likely to be symmetrical, affecting both sides of the body. The joint may be warm and red.
With OA, symptoms may progress rapidly or they may develop over several years, depending on the individual. They can worsen and then remain stable for a long time, and they can vary by days. Factors that may cause them to worsen include cold weather, stress, and excessive activity.
With RA, symptoms usually appear over several weeks, but they can develop or worsen in a few days. A flare can happen when disease activity increases. Triggers vary, but they include changes in medication.
With OA, this can be:
- hard swelling, due to the formation of bone spurs
- soft swelling, as inflammation causes extra fluid to collect around the joint
Swelling may be more noticeable after a long period of inactivity, like when you first wake up in the morning.
This is because RA is a systemic disease, which means it affects the whole body. OA, meanwhile, only has a direct impact on the affected joint.
Exercise: Rx For Overcoming Osteoarthritis
Exercising may be the last thing you want to do when your joints are stiff and achy. But exercise is a crucial part of osteoarthritis treatment in order to ease pain and stay active.
Osteoarthritis is a chronic and progressive disease characterized by loss of the cartilage that covers and protects the ends of the bones where they meet at a joint. Without this protective coating, bone rubs against bone, causing irritation and inflammation. The result is pain and stiffness in the joint and often pain in the muscles and ligaments that surround it.
Osteoarthritis is the leading cause of disability in the United States. Nearly equal numbers of women and men have the condition, but women tend to develop symptoms after age 55, about 10 years later than men do. It most often affects the hips, knees, spine, and hands.
Because most people diagnosed with osteoarthritis are older about half of those over 65 have it to some degree it’s long been considered a normal part of aging that reflects a lifetime of wear and tear on cartilage. But experts now know that many factors besides age are involved. Osteoarthritis risk can be inherited. An injury or disease may also kick off the deterioration. The rate of progression depends on genetics, biomechanical forces, and biological and chemical processes, all of which vary from person to person.
Recommended Reading: Why Do My Knees Hurt When Its Cold
Youre Ignoring Depression Which Can Worsen Pain
Depression, sleep problems, and osteoarthritis pain appear to be linked, according to a study published in March 2015 in the journal Arthritis Care & Research that assessed sleep, pain, and depression symptoms in 288 adults over the course of a year. The anxiety, stress, and worry that can go along with someone whos depressed may minimize their ability to cope with osteoarthritis, Johnson says. If you think you may be depressed, seek treatment immediately.
Physical Therapy For Knee Osteoarthritis
Strengthening Exercises and Other Osteoarthritis Treatments
Physical therapy can be your first line of defense for managing knee OA symptoms.
Having knee osteoarthritis can sometimes seem like a double-edge sword. Overusing your knees can worsen your joint health and knee OA, but the less you move your knees, the weaker they can get. You need to find that balance of keeping your knee joints moving just enough so they’re strong and healthy, and physical therapy helps you do that.
With knee OA, the muscles surrounding the knee can become weak, and the knee joints can become stiff. This makes it difficult to do everyday tasks, such as walking or getting out of bed.
Physical therapy can help to reduce the pain, swelling, and stiffness of knee osteoarthritis, and it can help improve knee joint function. It can also make it easier for you to walk, bend, kneel, squat, and sit. In fact, a 2000 study found that a combination of manual physical therapy and supervised exercise has functional benefits for patients with knee osteoarthritis and may delay or prevent the need for surgery.1
Common Passive Treatments for Knee Osteoarthritis
Common Active Treatments for Knee Osteoarthritis
Both strengthening and flexibility exercises are important to do because they can help take strain off the knee. Learn more about exercise for knee osteoarthritis in our article about exercising to manage knee osteoarthritis.
Also Check: Inversion Table Knees
Cracking Or Popping Sounds
When you bend or straighten your knee, you may feel a grinding sensation or hear cracking or popping sounds. Doctors call this crepitus.
These symptoms can occur when youve lost some of the cartilage that helps with smooth range of motion. Both OA and RA can result in cartilage damage.
When cartilage is damaged, rough surfaces and bone spurs develop. As you move your joints, these rub against each other.
Running Safely With Knee Osteoarthritis
Knee osteoarthritis doesnt have to stop you from running when done carefully, it can actually reduce pain associated with arthritis.
Many people mistakenly believe that running causes knee osteoarthritis however, doctors now know this is not true. Researchers who compared long-term effects of walking, running and other strenuous forms of exercise found that running significantly decreased the risk of hip and knee replacement, while other forms of exercise increased it. Another long-term study of runners versus non-runners showed that the runners did not have a higher incidence of knee osteoarthritis than the non-runners.
While doctors are still trying to understand how running can improve knee arthritis directly, it is well understood that running can facilitate weight loss, which is known to significantly reduce stress on joints and improve OA symptoms.
Running can be a healthy way to manage symptoms of knee osteoarthritis, but there are a few considerations that should be made before you begin.
Take it Slowly, and Listen to your Body
Like with any new fitness program, its important to start slowly. D. Casey Kerrigan, MD, a pioneer of gait analysis research at Harvard University and owner of OESH Shoes, suggests working closely with your doctor and physical therapist, listening to your body and using pain as a signal to back off when youre pushing too hard. The goal is to run without knee pain. Build up to it, says Dr. Kerrigan.
Physical Activity
Read Also: What Do You Do For Water On The Knee
How Can I Prevent Osteoarthritis Of The Knee
While you cant always prevent osteoarthritis of the knee, there are steps you can take to reduce the risk youll develop it:
- Maintain a healthy weight.
- If you jog or run, do so on grass or soft surfaces.
- Vary your fitness routine with low-impact exercises such as swimming or cycling.
- Add light strength training to your fitness routine.
Deformities Of The Knee
The appearance of the knee can change during a flare and as damage progresses.
In RA, swelling and redness are common during a flare. In the long term, persistent inflammation can result in permanent damage to the cartilage and the tendons. This can affect the shape and appearance of the knee.
With OA, the muscles around the knee can weaken, resulting in a sunken appearance. The knees can start to point toward each other or bend outward.
Knee deformities range from barely noticeable to severe and debilitating.
Treatment will depend on the type of arthritis a person has.
Recommended Reading: Inversion Table After Hip Replacement
Do: Wear Comfortable Knee Joint
There are a fair number of studies that suggest shoe choice matters if you have knee osteoarthritis, Pisetsky says. In fact, flat, flexible shoes that mimic the foots natural mobility can decrease the force placed upon the knee during daily activities, according to a study published in the May 2013 issue of Arthritis and Rheumatology.
Pain From Osteoarthritis Of The Knee Is Caused By Changes In Synovial Fluid And Joint Structures
A healthy knee contains synovial fluid, a viscous liquid that is responsible for lubricating the joint and absorbing shocks. Hyaluronic acid is a major component of normal synovial fluid and contributes to the fluids viscoelastic properties. Pain from osteoarthritis of the knee is caused by changes in synovial fluid and joint structures.
Changes in the synovial fluid and degeneration of joint structures may lead to pain in people with osteoarthritis of the knee.
Changes in the synovial fluid and degeneration of joint structures may lead to pain in people with osteoarthritis of the knee.
You May Like: Can I Regrow Cartilage In My Knee
How To Use Pain Medications Properly
There are two types of over-the-counter pain medications that can be used for osteoarthritis. Acetaminophen is a pain reliever but not an anti-inflammatory. It may help with mild knee pain.
NSAIDs can be more effective because they both relieve pain and reduce inflammation. However, they come with potential side effects and risks. NSAIDs can irritate the lining of the stomach, which may lead to an ulcer or other stomach problems. They also can impair kidney function. Some NSAIDs can increase blood pressure. And theyve been linked to an increased risk for heart disease.
Because of the risks, Dr. Day cautions against using NSAIDs regularly over long periods of time. Instead, she uses NSAIDs for her patients in two ways. First, people who have a flare-up of pain can take them regularly for three to five days and then stop. Second, they can be used over the long term, but only occasionally, maybe a couple of times a week as needed.
If youre taking NSAIDs several times a day for long periods of time, Dr. Day advises reducing their use by maximizing the other treatment strategies. She also suggests trying a topical NSAID, such as diclofenac , which has fewer potential side effects.
Opioid pain relievers are discouraged for long-term treatment of chronic knee pain. The milder narcotic tramadol might be appropriate for occasional use in some people, says Dr. Day.
How Is It Diagnosed
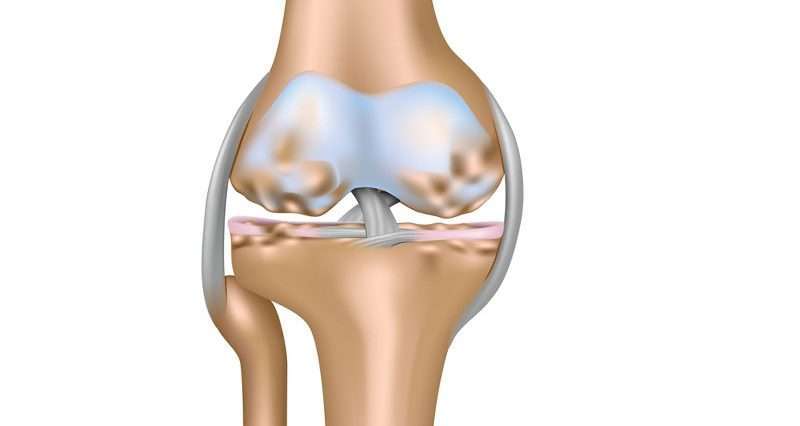
Knee OA is diagnosed by 2 primary processes. The first is based on your report of your symptoms and a clinical examination. Your physical therapist will ask you questions about your medical history and activity. The therapist will perform a physical exam to measure your knee’s movement , strength, mobility, and flexibility. You might also be asked to perform various movements to see if they increase or decrease the pain you are experiencing.
The second tool used to diagnose knee OA is diagnostic imaging. Your physical therapist may refer you to a physician, who will order X-rays of the knee in a variety of positions to check for damage to the bone and cartilage of your knee joint. If more severe joint damage is suspected, an MRI may be ordered to look more closely at the overall status of the joint and surrounding tissues. Blood tests also may be ordered to help rule out other conditions that can cause symptoms similar to knee OA.
You May Like: How To Whiten Knees And Elbows
How Does The Condition Change Over Time
The Kellgren-Lawrence Classification of Osteoarthritis is a common system for describing the stages of knee osteoarthritis. Kellgren-Lawrence classification measures the progression of knee osteoarthritis in terms of joint space narrowing . The stages range from 0 to stage 4 . When discussing late stage or advanced knee osteoarthritis, it is usually in reference to those at stage 3 or 4 of the Kellgren-Lawrence classification system.In late stage knee osteoarthritis, there is little to no separation between the bones remaining. This can lead to very different symptoms from those experienced by people at earlier stages of the condition. When these bones freely grate together they often cause more severe pain and stiffness. This also leads to reduced mobility in many cases.
How Does It Feel
Individuals who develop knee OA may experience a wide range of symptoms and limitations based on the progression of the disease. Pain occurs when the cartilage covering the bones of the knee joint wears down. Areas where the cartilage is worn down or damaged exposes the underlying bone. The exposure of the bone allows increased stress and compression to the cartilage, and at times bone-on-bone contact during movement, which can cause pain. Because the knee is a weight-bearing joint, your activity level, and the type and duration of your activities usually have a direct impact on your symptoms. Symptoms may be worse with weight-bearing activity, such as walking while carrying a heavy object.
Symptoms of knee OA may include:
- Worsening pain during or following activity, particularly with walking, climbing, or descending stairs, or moving from a sitting to standing position.
- Pain or stiffness after sitting with the knee bent or straight for a prolonged period of time.
- A feeling of popping, cracking, or grinding when moving the knee
- Swelling following activity.
- Tenderness to touch along the knee joint.
Also Check: Nano Knee Surgery Cost
Replacing All Of A Hip
|
Sometimes the whole hip joint must be replaced. The whole hip joint is the top of the thighbone and the surface of the socket into which the head of the thighbone fits. This procedure is called total hip replacement or total hip arthroplasty. The head of the thighbone is replaced with a ball-shaped part , made of metal. The prosthesis has a strong stem that fits within the center of the thighbone. The socket is replaced with a metal shell lined with durable plastic. |
Who Gets Osteoarthritis Of The Knee
Osteoarthritis is the most common type of arthritis. While it can occur even in young people, the chance of developing osteoarthritis rises after age 45. According to the Arthritis Foundation, more than 27 million people in the U.S. have osteoarthritis, with the knee being one of the most commonly affected areas. Women are more likely to have osteoarthritis than men.
Recommended Reading: Why Does My Knee Stiffen Up After Sitting
Physical Therapy Guide To Osteoarthritis Of The Knee
Read Time:
Osteoarthritis of the knee is the inflammation and wearing away of the cartilage on the bones that form the knee joint . The diagnosis of knee OA is based on 2 primary findings: radiographic evidence of changes in bone health , and an individual’s symptoms . Approximately 14 million people in the United States have symptomatic knee OA. Although more common in older adults, 2 million of the 14 million people with symptomatic knee OA were younger than 45 when diagnosed, and more than half were younger than 65. Physical therapists treat knee OA to reduce pain and improve range of motion.
Physical therapists are movement experts. They improve quality of life through hands-on care, patient education, and prescribed movement. You can contact a physical therapist directly for an evaluation. To find a physical therapist in your area, visit Find a PT.
What Causes Osteoarthritis Of The Knee
Osteoarthritis of the knee happens when your knee joint cartilage wears out or is damaged. Articular cartilage is tough, rubbery tissue on the ends of your bones that lets you bend and move. Meniscal cartilage absorbs shock from pressure on your knee.
Your cartilage is like your cars shock absorber, protecting your car from bumps and jolts. Drive on lots of rough roads, your shocks wear out fast. Drive on easy streets, your shocks last longer. You can wear out or damage your knee joint cartilage if:
- Youre overweight. If your body mass index is 30 or more, youre seven times more likely to develop osteoarthritis in your knee than someone with a lower BMI.
- You injure your knee or have an old knee injury.
- You frequently put stress on your knee at your job or playing sports.
- You inherited a tendency to develop osteoarthritis of the knee.
- You have crooked bones or joints, such as having knocked knees.
Also Check: Do Compression Sleeves Help With Knee Pain